- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
Woman Discovers She Was 4 Months Pregnant Days After Giving Birth—Doctor Explains How
Credits: Instagram & Canva
Dr Joe Whittington, who goes by Dr Joe on his social media platforms is a certified MD in Emergency Medicine based in Apple Valley, California is a social media medical educator. He uploads many real-life health-related stories and cases to educate general public about it. In one such videos, he featured a woman who just had her baby four days ago and found out that she was four months pregnant.
Is This Possible?
Dr Joe says, "technically, yes". This phenomenon is known as superfetation that occurs when a woman releases an egg and it gets fertilized and implanted after she is already pregnant.
He says, "Usually pregnancy changes such as hormonal changes, changes in the uterus, and the cervical mucous plug all work to prevent this. So superfetation is extremely rare with only about 10 documented cases. But, it is possible."
What Is Superfetation?
It is a rare phenomenon where a second pregnancy occurs alongside an existing one. This happens when another ovum or the egg is fertilized by sperm and implanted in the womb days or weeks later than the first one. Babies born from superfetation are often considered twins as they may be born on the same birth on the same day. However, not always does it happen. In the case that Dr Joe picked up, the baby had a difference of four months.
ALSO READ: Pregnancy Trimesters, Everything You Need To Know About It
So, How Does It Happen?
In humans, pregnancy occurs when an egg is fertilized by sperm and implants in the uterus. For superfetation to happen, a second egg must be fertilized and implanted separately while a pregnancy is already underway.
For this to occur, three highly unlikely events must take place:
Ovulation during an ongoing pregnancy – This is rare because pregnancy hormones typically prevent further ovulation.
Fertilization of the second egg – Once pregnant, a woman’s cervix forms a mucus plug that blocks sperm from entering, making fertilization extremely unlikely.
Implantation in an already pregnant uterus – Implantation requires specific hormonal changes that usually don’t occur once pregnancy has begun.
Additionally, a growing fetus takes up space, making it harder for another embryo to implant.
Because these conditions are so improbable, superfetation is considered nearly impossible in natural pregnancies. However, a few reported cases exist, primarily in women undergoing fertility treatments like in vitro fertilization (IVF). In such cases, an embryo is transferred into the uterus, but if ovulation unexpectedly occurs and the egg is fertilized, superfetation might happen a few weeks later.
Could There Be Any Complications?
The biggest complication with superfetation is premature birth. The baby maybe born before time and could have the following medical conditions:
- trouble breathing
- low birth weight
- movement and coordination problems
- difficulties with feeding
- brain hemorrhage or bleeding in the brain
- neonatal respiratory distress syndrome, which is a breathing disorder caused by underdeveloped lungs
Women too could have complication, which includes high blood pressure and protein in the urine, a condition called preeclampsia, and gestational diabetes.
India Makes Significant Progress In Maternal Care, Nutrition And Child Immunization: NFHS-6

Credit: PIB
India’s Ministry of Health and Family Welfare (MoHFW) has released the National Family Health Survey-6 (NFHS-6), showing major improvements in maternal healthcare, nutrition, immunization, and family planning across the country.
The nationwide survey, which covered nearly 6.79 lakh households across 715 districts, highlighted stronger healthcare access and improved outcomes for women and children in the country.
Key Findings of NFHS-6
The NFHS-6 was conducted during 2023-24 by MoHFW with the International Institute for Population Sciences (IIPS), Mumbai as the nodal agency.
Maternal Care
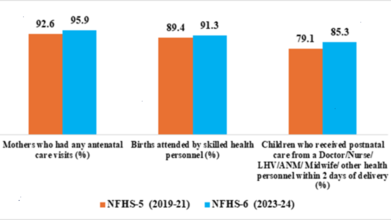
NFHS-6 recorded notable gains in maternal and child healthcare services nationwide. Nearly 96 per cent of pregnant women received antenatal care (ANC), while mothers receiving ANC during the first trimester increased from 70.0 per cent to 76.2 per cent.
The percentage of mothers receiving at least four ANC visits also rose from 58.5 per cent to 65.2 per cent, reflecting improved continuity of maternal healthcare services.
Institutional deliveries increased from 88.6 per cent to 90.6 per cent, bringing India closer to universal institutional delivery coverage.
Maternal nutrition indicators also improved significantly. Women consuming iron folic acid supplements for 100 days or more during pregnancy increased from 44.1 per cent to 54.9 per cent. Those consuming supplements for 180 days or more rose from 26.0 per cent to 37.8 per cent.
Family Planning
India’s Total Fertility Rate (TFR) remained stable at 2.0, while the Contraceptive Prevalence Rate (CPR) increased from 66.7 per cent to 69.1 per cent.
The findings reflect improved access to family planning services and the continued impact of government programs, including Mission Parivar Vikas.
Child Immunization
India also recorded progress towards universal immunization coverage. Full vaccination coverage among children aged 12-23 months increased from 83.8 per cent to 87.1 per cent based on vaccination cards.
More than 95 per cent of children received vaccinations through public health facilities, highlighting continued trust in the public healthcare system.
Coverage of major vaccines improved significantly. Rotavirus vaccination coverage surged from 36.4 per cent to 85.4 per cent, while coverage of the second dose of measles-containing vaccine increased from 58.6 per cent to 71.8 per cent.
The survey also found improvement in child health indicators. Symptoms of acute respiratory infection (ARI) among children declined from 2.8 per cent to 1.9 per cent, while severe diarrhea prevalence fell to 0.5 per cent.
The gains were attributed to stronger last-mile healthcare delivery, improved cold chain systems, digital tracking through U-WIN, and active community participation under the Universal Immunization Program.
Also read: Ebola: Inside India’s RT-PCR Tests For The Bundibugyo Strain| Explained
Child Nutrition Outcomes
NFHS-6 also reported encouraging progress in child nutrition indicators. More than 95 per cent of children under six months were breastfed during the survey period. The percentage of children breastfed within one hour of birth increased from 41.8 per cent to 50.1 per cent.
Stunting among children under five years declined sharply from 35.5 per cent to 29.3 per cent, indicating improvement in long-term nutritional outcomes.
Severe wasting declined from 7.7 per cent to 5.2 per cent, while underweight prevalence among children under five registered a marginal decline from 32.1 per cent to 31.8 per cent.
Infant and young child feeding practices also improved. Children aged 6-8 months receiving solid or semi-solid food along with breastmilk increased from 45.9 per cent to 59.5 per cent.
Down Syndrome Diagnosis: What Life Really Looks Like For Families
Credit: iStock
The birth of a child is often filled with joy, hope, and dreams for the future. But for some families, that journey also begins with an unexpected diagnosis — Down syndrome.
According to health experts, while the news can initially feel overwhelming, understanding the condition and accessing the right support can help children with Down syndrome lead fulfilling and meaningful lives.
Down syndrome, also known as Trisomy 21, is a genetic condition caused by the presence of an extra copy of chromosome 21. Instead of the usual 46 chromosomes, individuals with Down syndrome are born with 47. This additional chromosome can affect physical growth, learning, speech, and overall development.
Speaking to HealthandMe, Neurologist Dr. Rahul Chawla from ISIC Multispeciality Hospital says families often struggle emotionally after hearing the diagnosis, but understanding that Down syndrome is a genetic condition — and not a disease — can gradually help them move toward acceptance.
He noted that children with Down syndrome may learn and develop differently, but with proper medical care, therapy, emotional support, and inclusive education, many go on to study, work, play sports, and live independently with support.
How The Condition Is Diagnosed
Dr. Sweta Singla, Consultant and Head of Movement Disorder & Neurology at Manipal Hospitals, Dwarka, explained to HealthandMe that the condition can often be identified during pregnancy through screening tests such as blood tests and ultrasounds, and confirmed through diagnostic procedures like amniocentesis. After birth, genetic testing helps confirm the diagnosis.
The experts emphasized that early intervention plays a major role in improving quality of life.
"Physiotherapy, occupational therapy, and speech therapy started during infancy can help children develop communication and motor skills more effectively," Dr. Sweta said.
The experts warned that regular medical check-ups are important because children with Down syndrome may be more prone to conditions such as congenital heart defects, thyroid disorders, hearing difficulties, and vision problems.
Every Child Is Different
Children with Down syndrome present distinctive facial features, low muscle tone, delayed developmental milestones, short stature, and mild to moderate intellectual disability. Hearing and vision problems may also occur.
However, all children with Down syndrome have their own personalities, strengths, talents, and emotions, Prof. (Dr.) Brig. Ashok Saxena, Director of Neonatology and Paediatrics at ShardaCare–Healthcity, told HealthandMe.
Also read: Thyroid Disorders Affect Men Too: How They Impact Sperm Health
"Each child with Down syndrome is different – they all have their personalities, strengths, talents, and feelings," he said, adding that while some may take longer to learn speech, movement, or social skills, many are affectionate, emotionally expressive, and socially engaging.
Dr Ashok noted that a diagnosis of Down syndrome can be a very emotional and stressful time for parents.
"It can also be frightening, confusing, and filled with a lot of questions. It is important to keep in mind, though, that a diagnosis of Down syndrome doesn't mean a child's life ends. Children with Down syndrome can live a full and happy life with a loving family and appropriate medical treatment, emotional support, early therapies, and an inclusive environment," he said.
Breaking Stigma And Building Inclusion
Read More: Steroids During COVID Surging Hip Replacement Surgeries In Young Adults, Say Experts
Inclusive education and social acceptance are also considered essential.
The doctors noted that supportive teachers, accessible opportunities, and community awareness can help children gain confidence and independence.
Families are also encouraged to seek counselling and support groups to cope with emotional stress, fear, guilt, or social stigma that may accompany the diagnosis.
Medical professionals say that awareness around Down syndrome has improved significantly over the years, alongside advancements in healthcare and therapies that have enhanced life expectancy and quality of life.
Understanding Pediatric Blood Cancer: Symptoms Parents Should Know
Credit: iStock
Pediatric hematological malignancies, specifically leukemia and lymphoma, constitute some of the most frequently observed forms of cancer in pediatrics.
Pediatric cancers make up almost 7.9% of all cancers that are diagnosed in India, according to figures released by the Indian Council of Medical Research (ICMR).
Leukemia is responsible for almost half of all pediatric cancers in children under 14 years old.
Why Early Detection Matters: Common Symptoms
Healthcare professionals assert that early detection is essential in enhancing treatment success. Nevertheless, the symptoms are often mild and can be easily misdiagnosed as other childhood conditions.
Parents need to carefully observe any symptoms such as recurring fever, fatigue, susceptibility to infections, inexplicable bruising, and gum and nose bleeds. Pain in bones and joints, swelling in the lymph nodes, rapid weight loss, pale complexion, and protracted weakness are some other red flags that must not be overlooked.
Parents usually think these symptoms are associated with infections during the changing season or lack of nutrients in the body; however, if such symptoms do not subside within two weeks, medical attention is vital.
How Blood Cancer Affects The Body
The origins of blood cancer are found in bone marrow, causing problems with blood cell development. Symptoms can include anemia, which causes a low hemoglobin level, as well as low platelet levels and immune problems.
According to experts, a child suffering from blood cancer may also experience symptoms like fatigue and poor appetite.
Awareness Can Save Lives
Fortunately, good progress has been made in terms of survival rates for pediatric blood cancers through early diagnosis and new treatment techniques.
Research and professional opinions indicate that a significant number of kids who suffer from ALL, which is the most prevalent type of blood cancer among children, are able to enter long-lasting remission.
The importance of awareness among parents cannot be understated. Not every fever and bruise indicates cancer; however, symptoms that are seen are inexplicable and must always be taken into consideration. It is critical to consult an expert on time; this will definitely make a difference in treatment and recovery.
© 2024 Bennett, Coleman & Company Limited

