- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
The Life-Saving Surgery That Saved The Twin Brothers

Credits: King's College Hospital NHS Foundation Trust
Eight-month-old twins from Hayward Heath, West Sussex, recently met the surgeon who saved their lives even before they were born. The BBC reports how their mother, Katerina Ahouansou, at six months pregnant, during a routine scan, uncovered a serious issue with their development and blood supply.
Doctors diagnosed the twins with twin-to-twin transfusion syndrome or TTTS. It is a condition where one twin received more blood and nourishment than the other due to uneven blood vessel distribution in the placenta. In case there is no medical intervention, it could be fatal for both the twins.
A Specialist Steps In
This is when Ahouansou was referred to Professor Kypros Nicolaides at King’s College Hospital in London. Professor Nicolaides is a pioneer in fetal medicine and he specializes in a laser procedure that redistributes blood supply between twins in cases of TTTS.
When Ahouansou was scanned, Nicolaides observed that one of the twins were significantly smaller than the other. "There was a very high chance that if we did not intervene, both twins could die," he recalled.
An Operation No Less Than A Miracle
The life-saving laser surgery was performed and within a week the doctors saw an improvement with the twin who was smaller in size. When the twins were born, they weighed 1.5kg and 1.7kg. To recognize the efforts by the surgeon, Ahouansou named them Kai Kypros and Asher Nicolas after Professor Kypros Nicolaides.
Ahouansou also expressed deep gratitude for the professor's expertise and called him "proof that miracles can be performed by people who are devotees to their profession."
Professor Kypros Nicolaides has been at King’s College Hospital since 1980 and is widely regarded as a leader in fetal medicine. His groundbreaking research and development of screening and surgical techniques have saved countless lives.
Through his dedication, Professor Nicolaides has given many families hope, demonstrating how medical advancements continue to improve survival rates for complex fetal conditions like TTTS.
More about Twin-to-twin Transfusion Syndrome
As per the John Hopkins Medicine, TTTS is a rare pregnancy condition that affects identical twins or other multiples. It happens in pregnancies where twins share one placenta and a network of blood vessels that supply oxygen and nutrients essential for development in the womb. These pregnancies are known as monochorionic.
Sometimes, the blood vessels in the placenta are unevenly distributed, causing an imbalance in blood flow between the twins. The donor twin loses more blood than it receives, leading to malnutrition and potential organ failure. Meanwhile, the recipient twin gets an excess of blood, putting strain on the heart and increasing the risk of cardiac complications.
Impact on the Donor Twin
The donor twin loses blood volume (hypovolemia), reducing kidney function and urine production. This leads to low amniotic fluid levels (oligohydramnios) or, in severe cases, a complete absence (anhydramnios). Without proper blood circulation, the donor twin faces cardiovascular issues, increasing the risk of death.
Impact on the Recipient Twin
The recipient twin experiences excess blood volume (hypervolemia), causing increased urination and excessive amniotic fluid (polyhydramnios). The overworked heart struggles to handle the surplus blood, leading to cardiovascular dysfunction, heart failure, and, in extreme cases, death.
Introducing Eggs Before Age One May Lower Allergy Risk by 17%: Study

Credit: iStock
Eggs are a great source of protein. At the same time, they are one of the most common foods that cause allergies in children.
A new study conducted in Australia showed that introducing eggs to children before the age of one may reduce the risk of allergy by 17 per cent. The findings were published in the journal JAMA Pediatrics.
Jennifer Koplin, Associate Professor at the Child Health Research Centre at The University of Queensland, said: “Australia has one of the highest rates of food allergy in the world, with one in 10 infants allergic to one or more foods".
To curb the allergy rates, the Australian infant feeding guidelines, issued by the Australasian Society of Clinical Immunology and Allergy in 2016, revolutionized allergy prevention by advising parents to introduce well-cooked egg and smooth peanut butter soon after starting solid foods, generally around six months of age.
The research, led by a team from UQ and the Murdoch Children's Research Institute, examined 7,200 children in two Australian population-based studies to assess whether egg allergy rates had declined since the introduction of the guidelines. The risk of allergy decreased by 17 per cent among babies who started eating eggs early.
“Most parents followed the guidelines, and these results provide reassurance that this advice will help reduce the chance of their child developing an egg allergy,” Dr Koplin said.
Also read: I Ate Eggs And Toast For Breakfast Every Day—Here’s How My Body Reacted
Lesser Allergy In Infants With Eczema
According to Associate Professor Rachel Peters of the Murdoch Children's Research Institute, the reduction in egg allergy was more pronounced in babies with eczema, a known risk factor for food allergies. Among these children, egg allergy rates were reduced from 35 per cent to 22 per cent.
“The introduction of the 2016 guidelines was a major change from most advice given in the 1990s and early 2000s, which recommended parents delay giving eggs and other allergenic foods until 1–3 years of age if there was a strong family history of allergy,” Dr Peters said.
Allergenic Foods Before Age One
Other common allergy-causing foods, such as cow's milk, fish, sesame, wheat, and tree nuts, are also recommended to be included in a child's diet before one year of age. Dr Koplin, however, urged for more research into food allergies.
Read More: Eating Almonds Daily Can Prevent Cognitive Decline In Prediabetic Adults
Common Symptoms of Egg Allergy
According to the Mayo Clinic, egg allergy symptoms usually start a few minutes to a few hours after eating eggs or foods containing eggs. While egg allergies can occur as early as infancy, most children outgrow their egg allergy by age 16.
Egg allergy symptoms can include:
- Skin swelling or itchy bumps called hives — the most common egg allergy reaction.
- Stuffy or runny nose and sneezing, also known as allergic rhinitis.
- Digestive symptoms such as cramps, upset stomach and vomiting.
- Asthma symptoms such as coughing, wheezing, chest tightness or shortness of breath.
More Than Luck: Understanding The Roadmap After Repeated Miscarriages

Credit: Canva
Repeated miscarriages can cause stress and anxiety in couples who are searching for answers. Hence, understanding the possible causes, getting timely investigations, and following the right treatment roadmap can help improve the chances of a healthy pregnancy in the future.
Experiencing a miscarriage can be heartbreaking, but repeated miscarriages can feel even more overwhelming for couples trying to build a family. Many people believe pregnancy loss is simply due to bad luck or stress, but recurrent miscarriages often need proper medical evaluation to identify the underlying cause.
Couples tend to avoid seeking help for repeated miscarriages and keep blaming each other. However, with the help of awareness, timely testing, and the right support, many couples can go on to have successful pregnancies.
What Is Recurrent Pregnancy Loss?
Repeated miscarriage, also called recurrent pregnancy loss, refers to two or more consecutive pregnancy losses. While not every case has a clear explanation, several medical, genetic, hormonal, and lifestyle-related factors may contribute to repeated pregnancy failure.
Hence, couples will have to consult a fertility expert who will help them understand the causes behind the repeated miscarriages.
Why Medical Evaluation Is Important
The roadmap to finding answers: So, the repeated miscarriage will need a detailed medical evaluation of both partners. The expert will review previous pregnancy history, medical conditions, family history, lifestyle habits, and past test results. This helps identify possible patterns or hidden health concerns.
- Genetic testing may be advised because chromosome-related problems in either partner can increase the risk of miscarriage.
- Hormonal issues such as thyroid disorders, uncontrolled diabetes, or hormonal imbalance can also affect pregnancy health.
- In some women, structural problems in the uterus, such as fibroids, polyps, scar tissue, or an abnormal uterine shape, may interfere with implantation or fetal growth.
- Blood clotting disorders and immune-related conditions can also increase the risk of pregnancy loss.
Lifestyle Factors Matter Too
Smoking, alcohol, obesity, poor sleep, stress, and unhealthy eating habits may negatively affect fertility and pregnancy outcomes. Age can also influence egg quality and increase the chances of miscarriage.
Couples must seek timely help for repeated miscarriages, maintain an optimum weight, quit smoking and alcohol, and eat a balanced diet. Stay stress-free by doing yoga and meditation.
Exercise on a daily basis as advised by the expert, go for regular health check-ups and follow-ups with the doctor. Take prescribed supplements such as folic acid regularly. Follow these crucial tips, and it is possible to conceive even after facing repeated miscarriage.
India Makes Significant Progress In Maternal Care, Nutrition And Child Immunization: NFHS-6

Credit: PIB
India’s Ministry of Health and Family Welfare (MoHFW) has released the National Family Health Survey-6 (NFHS-6), showing major improvements in maternal healthcare, nutrition, immunization, and family planning across the country.
The nationwide survey, which covered nearly 6.79 lakh households across 715 districts, highlighted stronger healthcare access and improved outcomes for women and children in the country.
Key Findings of NFHS-6
The NFHS-6 was conducted during 2023-24 by MoHFW with the International Institute for Population Sciences (IIPS), Mumbai as the nodal agency.
Maternal Care
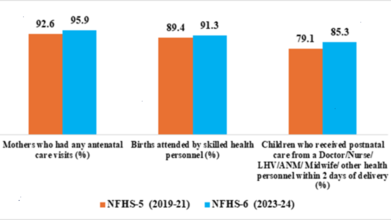
NFHS-6 recorded notable gains in maternal and child healthcare services nationwide. Nearly 96 per cent of pregnant women received antenatal care (ANC), while mothers receiving ANC during the first trimester increased from 70.0 per cent to 76.2 per cent.
The percentage of mothers receiving at least four ANC visits also rose from 58.5 per cent to 65.2 per cent, reflecting improved continuity of maternal healthcare services.
Institutional deliveries increased from 88.6 per cent to 90.6 per cent, bringing India closer to universal institutional delivery coverage.
Maternal nutrition indicators also improved significantly. Women consuming iron folic acid supplements for 100 days or more during pregnancy increased from 44.1 per cent to 54.9 per cent. Those consuming supplements for 180 days or more rose from 26.0 per cent to 37.8 per cent.
Family Planning
India’s Total Fertility Rate (TFR) remained stable at 2.0, while the Contraceptive Prevalence Rate (CPR) increased from 66.7 per cent to 69.1 per cent.
The findings reflect improved access to family planning services and the continued impact of government programs, including Mission Parivar Vikas.
Child Immunization
India also recorded progress towards universal immunization coverage. Full vaccination coverage among children aged 12-23 months increased from 83.8 per cent to 87.1 per cent based on vaccination cards.
More than 95 per cent of children received vaccinations through public health facilities, highlighting continued trust in the public healthcare system.
Coverage of major vaccines improved significantly. Rotavirus vaccination coverage surged from 36.4 per cent to 85.4 per cent, while coverage of the second dose of measles-containing vaccine increased from 58.6 per cent to 71.8 per cent.
The survey also found improvement in child health indicators. Symptoms of acute respiratory infection (ARI) among children declined from 2.8 per cent to 1.9 per cent, while severe diarrhea prevalence fell to 0.5 per cent.
The gains were attributed to stronger last-mile healthcare delivery, improved cold chain systems, digital tracking through U-WIN, and active community participation under the Universal Immunization Program.
Also read: Ebola: Inside India’s RT-PCR Tests For The Bundibugyo Strain| Explained
Child Nutrition Outcomes
NFHS-6 also reported encouraging progress in child nutrition indicators. More than 95 per cent of children under six months were breastfed during the survey period. The percentage of children breastfed within one hour of birth increased from 41.8 per cent to 50.1 per cent.
Stunting among children under five years declined sharply from 35.5 per cent to 29.3 per cent, indicating improvement in long-term nutritional outcomes.
Severe wasting declined from 7.7 per cent to 5.2 per cent, while underweight prevalence among children under five registered a marginal decline from 32.1 per cent to 31.8 per cent.
Infant and young child feeding practices also improved. Children aged 6-8 months receiving solid or semi-solid food along with breastmilk increased from 45.9 per cent to 59.5 per cent.
© 2024 Bennett, Coleman & Company Limited

