- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
Do Dads Experience Postpartum Depression?

Credits: Canva
By now, we all must be aware of how a mother's body changes during and even after pregnancy. What comes next is a challenging phase, called postpartum. However, it is not just the mothers, but dads too go through postpartum depression. As per the UT Southwestern Medical Center, 1 in 10 dads struggle with postpartum depression (PPD) and anxiety. According to a 2019 study published in Innovations in Clinical Neuroscience, a peer reviewed journal providing evidence-based information, titled Postpartum Depression in Men by Jonathan R Scarff defines postpartum depression as an episode of major depressive disorder occurring soon after the birth of a child. While it is frequently reported in mothers, but can also occur in father. However, there is no established criteria for this in men, although it could present over the course of a year, with symptoms of irritability restrict emotions, and depression.
Why Do Dads Experience PPD?
Fathers can also experience postpartum depression (PPD) due to various factors, including a history of depression, relationship conflicts, financial stress, and maternal depression. Sleep deprivation and disrupted circadian rhythms, known to affect maternal mental health, may also contribute to PPD in men. Additionally, hormonal changes during and after pregnancy play a role. Studies suggest that lower testosterone levels in new fathers reduce aggression and enhance responsiveness to a baby’s cries, while increased estrogen levels promote more engaged parenting. However, these hormonal shifts can also increase vulnerability to depression. Low testosterone is directly linked to depressive symptoms, and imbalances in estrogen, prolactin, vasopressin, and cortisol may hinder father-infant bonding, further exacerbating PPD symptoms.
In fact the study also goes on to note that fathers can experience prenatal depression like mothers too. While it depends on the kind of environment they are in, here are some of the common reasons why dads feel this way:
Hormonal Changes: As per a 2014 study published in the American Journal of Human Biology, titled Prenatal hormones in first-time expectant parents: Longitudinal changes and within-couple correlations, showed that fathers experience hormonal changes during and after their partner's pregnancy. The main reason is the decline in testosterone.
Feeling Disconnected: While dads also want to be part of the newborn experience, the baby usually spends most of the time with the mother. It may make them feel like they are on the "outside".
Other reasons include the pressure that a father feels. Parenting is not easy, it adds on to financial pressure, and this thought could also lead to depression. Especially, if depression runs in father's family, he is more likely to feel depressed with these changes around him. Most new parents underestimate the role lack of sleep plays in their lives. Staying up all night trying to get your baby to eat or sleep can leave you feeling sleep deprived, which could be one of the reasons why the father too may feel tired and depressed.
What Can Be Done?
The American Academy of Pediatrics recommended that postpartum depression screenings not be solely the responsibility of obstetrician, and it must be done by pediatricians too to incorporate maternal health. However, fathers too should go for such screenings. In fact, in 2020, an editorial in the Journal of the American Academy of Pediatrics called on pediatricians to assess the mental health of all new parents regardless of gender.
The ray of hope here is that more and more people are talking about it and are able to recognize the depression dads also go through. The change is not just for moms, but also for dads, thus it is important that they also are taken care of.
More Than Luck: Understanding The Roadmap After Repeated Miscarriages

Credit: Canva
Repeated miscarriages can cause stress and anxiety in couples who are searching for answers. Hence, understanding the possible causes, getting timely investigations, and following the right treatment roadmap can help improve the chances of a healthy pregnancy in the future.
Experiencing a miscarriage can be heartbreaking, but repeated miscarriages can feel even more overwhelming for couples trying to build a family. Many people believe pregnancy loss is simply due to bad luck or stress, but recurrent miscarriages often need proper medical evaluation to identify the underlying cause.
Couples tend to avoid seeking help for repeated miscarriages and keep blaming each other. However, with the help of awareness, timely testing, and the right support, many couples can go on to have successful pregnancies.
What Is Recurrent Pregnancy Loss?
Repeated miscarriage, also called recurrent pregnancy loss, refers to two or more consecutive pregnancy losses. While not every case has a clear explanation, several medical, genetic, hormonal, and lifestyle-related factors may contribute to repeated pregnancy failure.
Hence, couples will have to consult a fertility expert who will help them understand the causes behind the repeated miscarriages.
Why Medical Evaluation Is Important
The roadmap to finding answers: So, the repeated miscarriage will need a detailed medical evaluation of both partners. The expert will review previous pregnancy history, medical conditions, family history, lifestyle habits, and past test results. This helps identify possible patterns or hidden health concerns.
- Genetic testing may be advised because chromosome-related problems in either partner can increase the risk of miscarriage.
- Hormonal issues such as thyroid disorders, uncontrolled diabetes, or hormonal imbalance can also affect pregnancy health.
- In some women, structural problems in the uterus, such as fibroids, polyps, scar tissue, or an abnormal uterine shape, may interfere with implantation or fetal growth.
- Blood clotting disorders and immune-related conditions can also increase the risk of pregnancy loss.
Lifestyle Factors Matter Too
Smoking, alcohol, obesity, poor sleep, stress, and unhealthy eating habits may negatively affect fertility and pregnancy outcomes. Age can also influence egg quality and increase the chances of miscarriage.
Couples must seek timely help for repeated miscarriages, maintain an optimum weight, quit smoking and alcohol, and eat a balanced diet. Stay stress-free by doing yoga and meditation.
Exercise on a daily basis as advised by the expert, go for regular health check-ups and follow-ups with the doctor. Take prescribed supplements such as folic acid regularly. Follow these crucial tips, and it is possible to conceive even after facing repeated miscarriage.
India Makes Significant Progress In Maternal Care, Nutrition And Child Immunization: NFHS-6

Credit: PIB
India’s Ministry of Health and Family Welfare (MoHFW) has released the National Family Health Survey-6 (NFHS-6), showing major improvements in maternal healthcare, nutrition, immunization, and family planning across the country.
The nationwide survey, which covered nearly 6.79 lakh households across 715 districts, highlighted stronger healthcare access and improved outcomes for women and children in the country.
Key Findings of NFHS-6
The NFHS-6 was conducted during 2023-24 by MoHFW with the International Institute for Population Sciences (IIPS), Mumbai as the nodal agency.
Maternal Care
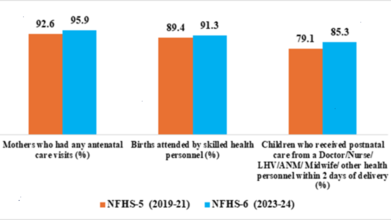
NFHS-6 recorded notable gains in maternal and child healthcare services nationwide. Nearly 96 per cent of pregnant women received antenatal care (ANC), while mothers receiving ANC during the first trimester increased from 70.0 per cent to 76.2 per cent.
The percentage of mothers receiving at least four ANC visits also rose from 58.5 per cent to 65.2 per cent, reflecting improved continuity of maternal healthcare services.
Institutional deliveries increased from 88.6 per cent to 90.6 per cent, bringing India closer to universal institutional delivery coverage.
Maternal nutrition indicators also improved significantly. Women consuming iron folic acid supplements for 100 days or more during pregnancy increased from 44.1 per cent to 54.9 per cent. Those consuming supplements for 180 days or more rose from 26.0 per cent to 37.8 per cent.
Family Planning
India’s Total Fertility Rate (TFR) remained stable at 2.0, while the Contraceptive Prevalence Rate (CPR) increased from 66.7 per cent to 69.1 per cent.
The findings reflect improved access to family planning services and the continued impact of government programs, including Mission Parivar Vikas.
Child Immunization
India also recorded progress towards universal immunization coverage. Full vaccination coverage among children aged 12-23 months increased from 83.8 per cent to 87.1 per cent based on vaccination cards.
More than 95 per cent of children received vaccinations through public health facilities, highlighting continued trust in the public healthcare system.
Coverage of major vaccines improved significantly. Rotavirus vaccination coverage surged from 36.4 per cent to 85.4 per cent, while coverage of the second dose of measles-containing vaccine increased from 58.6 per cent to 71.8 per cent.
The survey also found improvement in child health indicators. Symptoms of acute respiratory infection (ARI) among children declined from 2.8 per cent to 1.9 per cent, while severe diarrhea prevalence fell to 0.5 per cent.
The gains were attributed to stronger last-mile healthcare delivery, improved cold chain systems, digital tracking through U-WIN, and active community participation under the Universal Immunization Program.
Also read: Ebola: Inside India’s RT-PCR Tests For The Bundibugyo Strain| Explained
Child Nutrition Outcomes
NFHS-6 also reported encouraging progress in child nutrition indicators. More than 95 per cent of children under six months were breastfed during the survey period. The percentage of children breastfed within one hour of birth increased from 41.8 per cent to 50.1 per cent.
Stunting among children under five years declined sharply from 35.5 per cent to 29.3 per cent, indicating improvement in long-term nutritional outcomes.
Severe wasting declined from 7.7 per cent to 5.2 per cent, while underweight prevalence among children under five registered a marginal decline from 32.1 per cent to 31.8 per cent.
Infant and young child feeding practices also improved. Children aged 6-8 months receiving solid or semi-solid food along with breastmilk increased from 45.9 per cent to 59.5 per cent.
Down Syndrome Diagnosis: What Life Really Looks Like For Families
Credit: iStock
The birth of a child is often filled with joy, hope, and dreams for the future. But for some families, that journey also begins with an unexpected diagnosis — Down syndrome.
According to health experts, while the news can initially feel overwhelming, understanding the condition and accessing the right support can help children with Down syndrome lead fulfilling and meaningful lives.
Down syndrome, also known as Trisomy 21, is a genetic condition caused by the presence of an extra copy of chromosome 21. Instead of the usual 46 chromosomes, individuals with Down syndrome are born with 47. This additional chromosome can affect physical growth, learning, speech, and overall development.
Speaking to HealthandMe, Neurologist Dr. Rahul Chawla from ISIC Multispeciality Hospital says families often struggle emotionally after hearing the diagnosis, but understanding that Down syndrome is a genetic condition — and not a disease — can gradually help them move toward acceptance.
He noted that children with Down syndrome may learn and develop differently, but with proper medical care, therapy, emotional support, and inclusive education, many go on to study, work, play sports, and live independently with support.
How The Condition Is Diagnosed
Dr. Sweta Singla, Consultant and Head of Movement Disorder & Neurology at Manipal Hospitals, Dwarka, explained to HealthandMe that the condition can often be identified during pregnancy through screening tests such as blood tests and ultrasounds, and confirmed through diagnostic procedures like amniocentesis. After birth, genetic testing helps confirm the diagnosis.
The experts emphasized that early intervention plays a major role in improving quality of life.
"Physiotherapy, occupational therapy, and speech therapy started during infancy can help children develop communication and motor skills more effectively," Dr. Sweta said.
The experts warned that regular medical check-ups are important because children with Down syndrome may be more prone to conditions such as congenital heart defects, thyroid disorders, hearing difficulties, and vision problems.
Every Child Is Different
Children with Down syndrome present distinctive facial features, low muscle tone, delayed developmental milestones, short stature, and mild to moderate intellectual disability. Hearing and vision problems may also occur.
However, all children with Down syndrome have their own personalities, strengths, talents, and emotions, Prof. (Dr.) Brig. Ashok Saxena, Director of Neonatology and Paediatrics at ShardaCare–Healthcity, told HealthandMe.
Also read: Thyroid Disorders Affect Men Too: How They Impact Sperm Health
"Each child with Down syndrome is different – they all have their personalities, strengths, talents, and feelings," he said, adding that while some may take longer to learn speech, movement, or social skills, many are affectionate, emotionally expressive, and socially engaging.
Dr Ashok noted that a diagnosis of Down syndrome can be a very emotional and stressful time for parents.
"It can also be frightening, confusing, and filled with a lot of questions. It is important to keep in mind, though, that a diagnosis of Down syndrome doesn't mean a child's life ends. Children with Down syndrome can live a full and happy life with a loving family and appropriate medical treatment, emotional support, early therapies, and an inclusive environment," he said.
Breaking Stigma And Building Inclusion
Read More: Steroids During COVID Surging Hip Replacement Surgeries In Young Adults, Say Experts
Inclusive education and social acceptance are also considered essential.
The doctors noted that supportive teachers, accessible opportunities, and community awareness can help children gain confidence and independence.
Families are also encouraged to seek counselling and support groups to cope with emotional stress, fear, guilt, or social stigma that may accompany the diagnosis.
Medical professionals say that awareness around Down syndrome has improved significantly over the years, alongside advancements in healthcare and therapies that have enhanced life expectancy and quality of life.
© 2024 Bennett, Coleman & Company Limited

