- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
Breastfeeding Week: Experts Share How Breastfeeding Helps You and Your Child?

Credits: Unsplash
World Breastfeeding Week (WBW), held in the first week of August every year, is a global campaign supported by the World Health Organisation and UNICEF and many Ministries of Health and civil society partners on the protection, promotion and support of breastfeeding. This initiative was started in 1992 to encourage mothers to breastfeed their children and build a support community for new mothers who face any difficulties in breastfeeding.
Why Did We Need An Awareness Week?
Dr Sangeetha Rao TP, consultant obstetrician and gynaecologist who has been practising for the last 13 years says that due to the lack of support from healthcare providers or family, physical challenges like latching difficulties, societal pressures, and misinformation around breastfeeding, many mothers stopped breastfeeding their babies. “Mothers often have the perception that their infant is not satisfied by breast milk alone. Mothers' concerns about lactation and nutrition issues are the most frequently cited reasons for stopping breastfeeding during the first two months,” says Dr Nisha Kapoor, who is the Director and Head of the Department of Obstetrics, Gynaecology and Minimally Invasive Laparoscopic and Robotic Surgery at Marengo Asia Hospitals.Gynaecologist, obstetrician and founder of Baby Soon Fertility and IVF Center, Dr Jyoti Bali with 26 years of experience says, “A reason why some mothers stopped breastfeeding was because of the increased marketing of formula as a convenient solution compared to breastfeeding.”
Experts agree that women undergo physical changes in their bodies during their pregnancy and while breastfeeding too, however, these have been exaggerated. “Breastfeeding can lead to temporary changes in breast size and shape, but these changes are typically normal and revert to baseline after weaning. Perceptions about breastfeeding causing long-term body changes are often unscientific or exaggerated,” says Dr Rao.
These were some of the reasons why women stopped breastfeeding and thus an initiative like World Breastfeeding Week was started. This also aims to highlight the health benefits to the mother and the child on breastfeeding.
Benefits of Breastfeeding on Mother
Breastfeeding is one of the most effective ways to ensure a child's health and survival. As per WHO, moms should initiate breastfeeding within the first hour of birth and continue breastfeeding for the first 6 months.Rao says that for the mother, it helps in faster postpartum recovery, reduces the risk of certain cancers, and can help with postpartum weight loss.
“Breast Feeding helps the mothers to shed their pregnancy weight more quickly because the production of milk requires the burning of calories,” agrees Dr Bali.
Other health benefits to mothers are postpartum healing, bonding with the baby and a decrease in the risk of ovarian cancer, mentions Dr Bali.
Breastfeeding Benefits on Baby
“IgA, IgG, and IgM are among the special proteins and antibodies found in breast milk that are absent from baby formulae. By covering the lining of the baby's developing intestines, these immunoglobulins provide passive immunity, shielding the youngster from potential infections and pathogens,” says Dr Neerja Goel, a senior obstetrician and gynaecologist with 45 years of experience.There are also nutritional values that help a preterm baby in his or her development. “For example, breast milk's higher protein content makes it easier for premature babies to absorb and digest than formula, which encourages better weight gain. Premature babies often have specific nutritional needs due to their early birth. Breast milk provides a tailored balance of proteins, fats, and carbohydrates that support their rapid growth and development. The composition of breast milk adjusts to meet the changing needs of a preterm infant, including higher levels of certain nutrients,” says Dr Goel.
Dr Bali also points out that breast milk contains antibodies, probiotics and DHA and ARA, a kind of fatty acids that are required for brain development. Thus, a baby can benefit a great deal from breastfeeding.
Health Risks When Not Breastfeeding
“Infants, not being breastfed is associated with an increased incidence of infectious morbidity as well as elevated risks of childhood obesity and diabetes. For mothers, failure to breastfeed is associated with an increased incidence of premenopausal breast cancer, ovarian cancer, retained gestational weight gain, Type 2 diabetes, and metabolic syndrome,” points out Dr Ashutosh Sarwa, a health expert in Maternal, Newborn and Child Health & Nutrition at Nutrition International.Poor breastfeeding practices in infancy and early childhood, resulting in malnutrition, contribute to impaired cognitive and social development, poor school performance and reduced productivity in later life.
Sarwa points out that psychological factors like stress, anxiety, postpartum depression, poor latch due to anatomical issues or improper positioning, and other medical conditions are the common reasons for this. “Identification and management of the specific cause, appropriate counselling by a healthcare provider, support (emotional and workplace both) and alternative feeding options,” he says.
Unable To Breastfeed Your Child? Here is What You Can Do
There are now Breastmilk banks which can provide breast milk for your child. Breastmilk banks provide a vital resource for infants who cannot receive breast milk from their mothers, such as preterm or ill babies.Do not be worried about its safety, Dr Rao says that donated milk is screened, pasteurised, and distributed to ensure safety and nutrition.
Are You a Working Mother?
Breastfeeding can be successfully managed for a working mother who must spend lengthy hours away from her child by combining pumping and conserving breast milk.“Purchasing a superior electric breast pump can increase the effectiveness of the procedure. Maintaining a consistent pumping schedule—ideally, every three to four hours—helps keep the milk supply steady. Pumped milk can be refrigerated for up to four days if stored in sterile containers or bags that have been labelled with the date and time. Milk can be frozen and thawed for extended storage,” suggests Dr Goel.
More Than Luck: Understanding The Roadmap After Repeated Miscarriages

Credit: Canva
Repeated miscarriages can cause stress and anxiety in couples who are searching for answers. Hence, understanding the possible causes, getting timely investigations, and following the right treatment roadmap can help improve the chances of a healthy pregnancy in the future.
Experiencing a miscarriage can be heartbreaking, but repeated miscarriages can feel even more overwhelming for couples trying to build a family. Many people believe pregnancy loss is simply due to bad luck or stress, but recurrent miscarriages often need proper medical evaluation to identify the underlying cause.
Couples tend to avoid seeking help for repeated miscarriages and keep blaming each other. However, with the help of awareness, timely testing, and the right support, many couples can go on to have successful pregnancies.
What Is Recurrent Pregnancy Loss?
Repeated miscarriage, also called recurrent pregnancy loss, refers to two or more consecutive pregnancy losses. While not every case has a clear explanation, several medical, genetic, hormonal, and lifestyle-related factors may contribute to repeated pregnancy failure.
Hence, couples will have to consult a fertility expert who will help them understand the causes behind the repeated miscarriages.
Why Medical Evaluation Is Important
The roadmap to finding answers: So, the repeated miscarriage will need a detailed medical evaluation of both partners. The expert will review previous pregnancy history, medical conditions, family history, lifestyle habits, and past test results. This helps identify possible patterns or hidden health concerns.
- Genetic testing may be advised because chromosome-related problems in either partner can increase the risk of miscarriage.
- Hormonal issues such as thyroid disorders, uncontrolled diabetes, or hormonal imbalance can also affect pregnancy health.
- In some women, structural problems in the uterus, such as fibroids, polyps, scar tissue, or an abnormal uterine shape, may interfere with implantation or fetal growth.
- Blood clotting disorders and immune-related conditions can also increase the risk of pregnancy loss.
Lifestyle Factors Matter Too
Smoking, alcohol, obesity, poor sleep, stress, and unhealthy eating habits may negatively affect fertility and pregnancy outcomes. Age can also influence egg quality and increase the chances of miscarriage.
Couples must seek timely help for repeated miscarriages, maintain an optimum weight, quit smoking and alcohol, and eat a balanced diet. Stay stress-free by doing yoga and meditation.
Exercise on a daily basis as advised by the expert, go for regular health check-ups and follow-ups with the doctor. Take prescribed supplements such as folic acid regularly. Follow these crucial tips, and it is possible to conceive even after facing repeated miscarriage.
India Makes Significant Progress In Maternal Care, Nutrition And Child Immunization: NFHS-6

Credit: PIB
India’s Ministry of Health and Family Welfare (MoHFW) has released the National Family Health Survey-6 (NFHS-6), showing major improvements in maternal healthcare, nutrition, immunization, and family planning across the country.
The nationwide survey, which covered nearly 6.79 lakh households across 715 districts, highlighted stronger healthcare access and improved outcomes for women and children in the country.
Key Findings of NFHS-6
The NFHS-6 was conducted during 2023-24 by MoHFW with the International Institute for Population Sciences (IIPS), Mumbai as the nodal agency.
Maternal Care
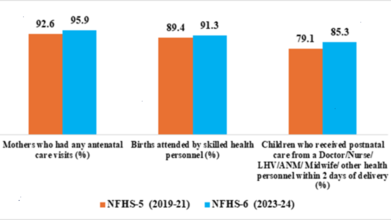
NFHS-6 recorded notable gains in maternal and child healthcare services nationwide. Nearly 96 per cent of pregnant women received antenatal care (ANC), while mothers receiving ANC during the first trimester increased from 70.0 per cent to 76.2 per cent.
The percentage of mothers receiving at least four ANC visits also rose from 58.5 per cent to 65.2 per cent, reflecting improved continuity of maternal healthcare services.
Institutional deliveries increased from 88.6 per cent to 90.6 per cent, bringing India closer to universal institutional delivery coverage.
Maternal nutrition indicators also improved significantly. Women consuming iron folic acid supplements for 100 days or more during pregnancy increased from 44.1 per cent to 54.9 per cent. Those consuming supplements for 180 days or more rose from 26.0 per cent to 37.8 per cent.
Family Planning
India’s Total Fertility Rate (TFR) remained stable at 2.0, while the Contraceptive Prevalence Rate (CPR) increased from 66.7 per cent to 69.1 per cent.
The findings reflect improved access to family planning services and the continued impact of government programs, including Mission Parivar Vikas.
Child Immunization
India also recorded progress towards universal immunization coverage. Full vaccination coverage among children aged 12-23 months increased from 83.8 per cent to 87.1 per cent based on vaccination cards.
More than 95 per cent of children received vaccinations through public health facilities, highlighting continued trust in the public healthcare system.
Coverage of major vaccines improved significantly. Rotavirus vaccination coverage surged from 36.4 per cent to 85.4 per cent, while coverage of the second dose of measles-containing vaccine increased from 58.6 per cent to 71.8 per cent.
The survey also found improvement in child health indicators. Symptoms of acute respiratory infection (ARI) among children declined from 2.8 per cent to 1.9 per cent, while severe diarrhea prevalence fell to 0.5 per cent.
The gains were attributed to stronger last-mile healthcare delivery, improved cold chain systems, digital tracking through U-WIN, and active community participation under the Universal Immunization Program.
Also read: Ebola: Inside India’s RT-PCR Tests For The Bundibugyo Strain| Explained
Child Nutrition Outcomes
NFHS-6 also reported encouraging progress in child nutrition indicators. More than 95 per cent of children under six months were breastfed during the survey period. The percentage of children breastfed within one hour of birth increased from 41.8 per cent to 50.1 per cent.
Stunting among children under five years declined sharply from 35.5 per cent to 29.3 per cent, indicating improvement in long-term nutritional outcomes.
Severe wasting declined from 7.7 per cent to 5.2 per cent, while underweight prevalence among children under five registered a marginal decline from 32.1 per cent to 31.8 per cent.
Infant and young child feeding practices also improved. Children aged 6-8 months receiving solid or semi-solid food along with breastmilk increased from 45.9 per cent to 59.5 per cent.
Down Syndrome Diagnosis: What Life Really Looks Like For Families
Credit: iStock
The birth of a child is often filled with joy, hope, and dreams for the future. But for some families, that journey also begins with an unexpected diagnosis — Down syndrome.
According to health experts, while the news can initially feel overwhelming, understanding the condition and accessing the right support can help children with Down syndrome lead fulfilling and meaningful lives.
Down syndrome, also known as Trisomy 21, is a genetic condition caused by the presence of an extra copy of chromosome 21. Instead of the usual 46 chromosomes, individuals with Down syndrome are born with 47. This additional chromosome can affect physical growth, learning, speech, and overall development.
Speaking to HealthandMe, Neurologist Dr. Rahul Chawla from ISIC Multispeciality Hospital says families often struggle emotionally after hearing the diagnosis, but understanding that Down syndrome is a genetic condition — and not a disease — can gradually help them move toward acceptance.
He noted that children with Down syndrome may learn and develop differently, but with proper medical care, therapy, emotional support, and inclusive education, many go on to study, work, play sports, and live independently with support.
How The Condition Is Diagnosed
Dr. Sweta Singla, Consultant and Head of Movement Disorder & Neurology at Manipal Hospitals, Dwarka, explained to HealthandMe that the condition can often be identified during pregnancy through screening tests such as blood tests and ultrasounds, and confirmed through diagnostic procedures like amniocentesis. After birth, genetic testing helps confirm the diagnosis.
The experts emphasized that early intervention plays a major role in improving quality of life.
"Physiotherapy, occupational therapy, and speech therapy started during infancy can help children develop communication and motor skills more effectively," Dr. Sweta said.
The experts warned that regular medical check-ups are important because children with Down syndrome may be more prone to conditions such as congenital heart defects, thyroid disorders, hearing difficulties, and vision problems.
Every Child Is Different
Children with Down syndrome present distinctive facial features, low muscle tone, delayed developmental milestones, short stature, and mild to moderate intellectual disability. Hearing and vision problems may also occur.
However, all children with Down syndrome have their own personalities, strengths, talents, and emotions, Prof. (Dr.) Brig. Ashok Saxena, Director of Neonatology and Paediatrics at ShardaCare–Healthcity, told HealthandMe.
Also read: Thyroid Disorders Affect Men Too: How They Impact Sperm Health
"Each child with Down syndrome is different – they all have their personalities, strengths, talents, and feelings," he said, adding that while some may take longer to learn speech, movement, or social skills, many are affectionate, emotionally expressive, and socially engaging.
Dr Ashok noted that a diagnosis of Down syndrome can be a very emotional and stressful time for parents.
"It can also be frightening, confusing, and filled with a lot of questions. It is important to keep in mind, though, that a diagnosis of Down syndrome doesn't mean a child's life ends. Children with Down syndrome can live a full and happy life with a loving family and appropriate medical treatment, emotional support, early therapies, and an inclusive environment," he said.
Breaking Stigma And Building Inclusion
Read More: Steroids During COVID Surging Hip Replacement Surgeries In Young Adults, Say Experts
Inclusive education and social acceptance are also considered essential.
The doctors noted that supportive teachers, accessible opportunities, and community awareness can help children gain confidence and independence.
Families are also encouraged to seek counselling and support groups to cope with emotional stress, fear, guilt, or social stigma that may accompany the diagnosis.
Medical professionals say that awareness around Down syndrome has improved significantly over the years, alongside advancements in healthcare and therapies that have enhanced life expectancy and quality of life.
© 2024 Bennett, Coleman & Company Limited

