- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
When Ozempic And Wegovy Fail To Work- Why GLP-1 Drugs Aren’t The Magic Bullet For Everyone
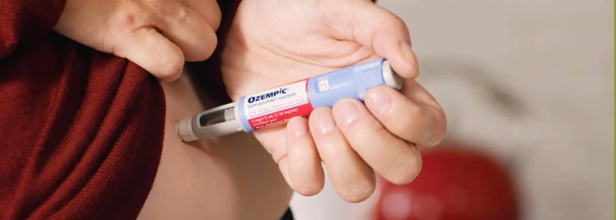
When Ozempic And Wegovy Fail To Work- Why GLP-1 Drugs Aren’t The Magic Bullet For Everyone
Ozempic and Wegovy have received a lot of publicity as revolutionizing treatment options for obesity. Both medications form a class of GLP-1 receptor agonists, which mimic a hormone in the body called glucagon-like peptide-1 and are involved in the regulation of appetite and blood sugar. Indeed, in initial clinical studies, the majority of those on the drugs lost 15% to 22% of body weight, hence much optimism. For most patients, these medications are underwhelming for about 20% of patients due to minimal weight loss or other challenges.
Take a closer look at why the weight loss drugs may not work for everyone, together with what options exist when they don't deliver the expected outcomes.
Why Weight Loss Drugs May Not Work
While GLP-1 receptor agonists have produced phenomenal responses in a majority of patients, it remains a reality that these drugs work differently for different people. Here's why:
1. Genetic and Hormonal Variability
Weight loss medications interact with complex systems in the body that differ from person to person. Genetics, hormones, and individual brain responses to energy regulation play significant roles in determining how a person responds to drugs like Ozempic and Wegovy.
2. Underlying Medical Conditions
Other conditions, such as sleep apnea, may be prevalent and prevent or delay the achievement of weight loss goals. Prescription drugs like antidepressants, steroids, or contraceptives are other medications that can nullify weight loss medication benefits.
3. Unrealistic Expectations
Often, they come to these medications with enormous hopes; expecting the promised rapid and dramatic weight loss. Progress creates disappointment if it has not stalled. In patients who rigidly follow recommended lifestyle modifications, frustration and disappointment are most common.
Why it is Important to Identify Non-responders
For most patients, the effectiveness of GLP-1 receptor agonists is evident within a few weeks of treatment. Weight loss typically begins within a few weeks of initiating therapy and tends to increase with dosage. However, some patients respond very little, if at all, despite strict adherence to their regimen.
For nonresponders, this can feel like a dead end. However, understanding the unique complexities of obesity is essential. This condition stems from brain dysfunction, and the pathways that contribute to weight regulation differ among individuals.
Alternative Treatment Options
When Ozempic or Wegovy doesn’t yield desired results, there are still many paths to explore:
1. Switching to Another GLP-1 Drug
For example, some patients who don't respond well to one GLP-1 receptor agonist might find success with another drug in the same class. Newer medications, such as Zepbound, target other hormone pathways and seem promising even for those not responsive to earlier drugs.
2. Use of Older Medications
While there is much to say about newer drugs, older treatments can still be useful and work for some patients. One can also seek the help of a medical provider specializing in obesity treatments in order to identify the best alternatives.
3. Lifestyle Changes
Diet, exercise, sleep, and stress management continue to be integral components of any weight loss program. New changes may be small but can make an enormous difference in one's health and success.
4. Medical Management of Obesity
It is a complex disorder, and most patients should receive a multidisciplinary treatment. Collaboration with an obesity-aware doctor may mean access to tailored treatment plans, ranging from psychological support all the way to metabolic testing, and many others.
Why Side Effects of Weight Loss Drug Ozempic May Be a Barrier
For others, side effects like nausea, vomiting, or diarrhea hinder them from continuing with these drugs. These symptoms often reduce as the body becomes accustomed, but for some, they might be severe enough to stop treatment altogether. In those instances, alternative drugs or procedures become vital to find.
Long-term effects of Ozempic or Wegovy on the Brain
Another largely unexplored area relates to GLP-1 drugs' long-term effects on the brain's regulation of hunger and satiety. Although GLP-1 drugs suppress appetite and can lead to effective weight loss, emerging research suggests that they may also affect brain reward mechanisms, changing the way patients experience foods.
This aspect could prove of paramount significance in the future treatment of obesity. Perhaps GLP-1 receptor agonists do indeed affect and rewire the brain's reward pathways and will thus provide sustained benefits beyond discontinuation. However, more research is required to understand this phenomenon fully.
While for many, Ozempic and Wegovy have revolutionized obesity treatment, these are certainly not a one size fits all. Nonresponders need not lose hope- alternative strategies and medications abound. A consultation with an obesity expert healthcare provider is essential to put together a comprehensive, tailored treatment plan.
The route toward effective weight loss may be challenging, but with the evolution of obesity medicine and a better understanding of individual needs, there is a path forward for everyone.
Can Herbs Help Reverse Early Liver Damage?

A healthy liver does not ask for much, just the right nutrition. (Photo credit: AI generated)
Many people follow what appears to be a reasonable eating pattern—meals at irregular hours, a light breakfast skipped in the name of time, and dinner pushed late into the evening. Yet the body, particularly the liver, does not respond well to such improvisation. What feels like a manageable routine on the surface can quietly accumulate into something more serious over months and years. The liver needs a consistent flow of nutrients to do its job, which includes managing blood sugar, breaking down fats, and supporting digestion. Long gaps between meals disrupt that rhythm.
Dr Babu U V, Director of R&D, Research & Development Centre, Himalaya Wellness Company, in an interview with Health and Me, spoke about the early symptoms of liver damage and explained how herbs can play a role in reversing it.
Symptoms of Early Liver Damage
Before most people realise that something is wrong with their liver, they may already be experiencing symptoms that indicate potential liver issues. These symptoms may include fatigue, bloating, digestive discomfort, or feeling heavy after eating. Most of the time, these signs are dismissed as minor concerns.
When these issues are ignored or go unnoticed, it becomes difficult to recognise that the liver may be weakened by stress and not functioning optimally. If these problems persist over time, fat can begin to accumulate in the liver, along with other types of metabolic imbalances throughout the body.
To restore balance in the body, small changes in daily habits can lead to significant improvements. For example, eating at regular intervals helps the body maintain a consistent metabolism. Similarly, having lighter dinners and avoiding late-night eating can support better digestion and metabolism of food.
Herbs That Strengthen Liver Health
Some herbs commonly used in Indian households and traditional medicine may help support the liver’s healing process, especially when it is under stress.
- Bhumi Amla (Bhumyamalaki) has been used for centuries in traditional remedies for liver health. It supports the body’s natural detoxification processes and liver function.
- Punarnava is another well-known herb that promotes both liver and kidney health. It is believed to help reduce inflammation and restore balance in the body.
- Turmeric (Haldi), found in almost every Indian kitchen, has anti-inflammatory and antioxidant properties. It supports metabolism and helps the body respond to oxidative stress.
- Chicory (Kasani) has long been associated with liver support. It helps the body manage toxin-related stress and supports overall liver function.
Each of these herbs works in different ways—some aid digestion, while others help neutralise free radicals and reduce oxidative stress—thereby supporting a healthier lifestyle.
The liver is highly resilient; however, it requires consistent care. An irregular dietary pattern may not affect the liver immediately, but over time it can have a significant impact. Paying attention to simple habits—such as when and how you eat—and choosing foods that support liver health can go a long way in maintaining optimal liver function over the long term.
World Liver Day 2026: Origin, Theme, and Significance
Credit: Canva
World Liver Day 2026 is observed every year on April 19 to raise awareness of the importance of liver health, focusing on preventing diseases such as cirrhosis and fatty liver through healthy lifestyles.
The liver is a key organ that filters blood, breaks down food, stores energy, and keeps the human body in balance.
However, rising metabolic risk factors, including high blood sugar and obesity, are increasingly driving cases of metabolic dysfunction-associated steatotic liver disease (MASLD).
Nearly one-third of the global adult population today lives with MASLD, which can remain asymptomatic for years but turn into deadly scarring (fibrosis), cirrhosis (advanced fibrosis and loss of some of the liver function), or even liver cancer.
World Liver Day: Origin
The European Association for the Study of the Liver (EASL) launched World Liver Day in 2010. The day was established on April 19 to commemorate the EASL's founding in 1966.
World Liver Day 2026: Theme
This year, 2026, the World Liver Day theme is “Solid Habits, Strong Liver”. It emphasizes building consistent lifestyle habits, such as balanced diet, regular exercise, avoiding alcohol, and routine check-ups, to strengthen liver health and prevent diseases.
Burden Of Liver Diseases
https://www.youtube.com/watch?v=zklb3ZCyX2o
From filtering toxins to aiding in digestion and metabolism, the liver silently performs over 500 crucial functions in the body. The organ is also blessed with the ability to regenerate itself.
Yet data shows that 2 million lives worldwide are lost each year to liver disease. About 1.5 billion people suffer from chronic liver disease.
MASLD, formerly known as non-alcoholic fatty liver disease (NAFLD), has emerged as the most common liver condition worldwide. These patients suffer from either obesity, diabetes, metabolic syndrome, hypertension, or cholesterol problems.
According to a recent study published in The Lancet Gastroenterology & Hepatology journal, MASLD affected 1.3 billion people around the globe in 2023.
The alarming study estimates the numbers to further spike by over 38 percent to reach 1.8 billion cases by 2050, causing substantial health and economic impacts worldwide.
MASLD remains one of the most prevalent and rapidly growing liver conditions worldwide, with its prevalence marking a 143 percent increase between 1990 and 2023.
Also read: Why Regular Scans Are Crucial for Liver Cancer Patients: Doctors Explain
People with obesity, diabetes, central or abdominal fat, dyslipidemia, hypertension, and insulin resistance are more likely to have MASLD. Obesity is the strongest risk factor, with the likelihood rising steeply from overweight to severe obesity.
Other signs to watch for include
- persistent fatigue
- Digestive issues and bloating
- Unexplained weight gain or difficulty losing weight
- Skin changes
Everyday Habits That Harm The Liver
Certain lifestyle choices can accelerate liver damage, such as:
- Overeating processed or fried foods
- High sugar intake (soft drinks, sweets, desserts)
- Physical inactivity or prolonged sitting
- Ignoring health issues like diabetes or hypertension
- Crash dieting or taking unprescribed supplements.
How To Improve Liver Health?
Early screening and detection are key to prevent irreversible stages. Yet liver disease can be prevented with lifestyle changes such as:
- Eating a balanced diet with vegetables, fruits, whole grains, and lean protein
- Engaging in at least 30 minutes of exercise daily
- Staying hydrated to help the liver flush out toxins
- Avoiding alcohol and smoking
- Avoiding self-medication and unnecessary pills
- Getting routine health screenings.
Why Irritable Bowel Syndrome Is Rising Among Young Working Adults

Credit: Canva
A growing number of young professionals aged 18 to 30 are being diagnosed with Irritable Bowel Syndrome (IBS), a trend that is linked to the pressures and habits of modern life, said health experts today.
World Irritable Bowel Syndrome Day is held annually on April 19th to raise global awareness, reduce stigma, and support the roughly 700 million people worldwide suffering from the condition.
According to health experts, the combination of long hours in the office, irregular diets, high-stress levels, and lack of physical activity has paved the way for a lifestyle that is making young adults increasingly susceptible to developing symptoms related to their gut.
Speaking to HealthandMe, Dr. Nidhi Rawal, Consultant - Pediatric Gastroenterologist and Hepatologist, Rainbow Hospital, explained the major risk factors that are taking a visible toll on digestive health.
1. Chronic stress
Young professionals are faced with a fast-paced job environment full of obstacles and demands that they experience daily, along with performance pressure and increased digital overload; all of these factors can hurt the gut-brain axis.
When the gut-brain axis becomes disrupted, the motility and sensitivity of the digestive system can be affected, producing gut-related symptoms, such as abdominal discomfort, excessive gas, and changes in bowel movements.
2. Dietary habits
The increased reliance on processed foods, increased frequency of ordering takeout and fast food, excessive caffeine consumption, and irregular meal schedules can disrupt digestion and alter the balance of healthy vs unhealthy microbiota in the digestive tract.
3. Skipping meals
Skipping meals or eating a late dinner can also raise risk of IBS, and worsen symptoms.
4. Lack of physical activity
Being sedentary for long periods of time results in slowing the digestion process and therefore increases the risk of constipation and bloating.
5. Poor sleeping habits
Common among people in this age group, this also affect hormones and digestion negatively.
6. Better access to diagnostic tests
Better access to diagnostic tests and awareness are leading to an increase in diagnosis of the condition, that can also enable faster treatment and early recovery.
What Is IBS?
Irritable Bowel Syndrome (IBS) is a common but often overlooked gastrointestinal disorder, and less than 15 per cent get diagnosed.
Common symptoms include
- bloated abdomen,
- abdominal pain,
- gas,
- diarrhea,
- constipation.
Why IBS Symptoms Are Often Ignored
IBS remains undiagnosed for many years as people tend to normalize these symptoms over time or attribute them to "something they ate" or everyday stresses.
One reason for this delay in being diagnosed is that the symptoms occur intermittently.
It is also important to note that the presentation of these symptoms is inconsistent and unpredictable; there may be episodes where the IBS can last many days, and then completely resolve, thus providing a false sense of relief.
Therefore, many individuals choose to delay consulting with a physician due to their belief that the symptoms they are experiencing are not serious.
Another contributing factor is that there is still a degree of reluctance or discomfort associated with discussing problems related to the gastrointestinal tract openly; this only further complicates under-reporting statistics.
IBS is a functional disorder. Therefore, routine diagnostic testing will not reveal any visible abnormalities.
Many patients may assume that the symptoms they are experiencing are not "real" or are not significant enough to warrant seeking medical attention, even though the discomfort they experience can be quite significant and affect their daily lives.
To treat IBS effectively, those suffering from it need to adopt some lifestyle changes, such as
Regular mealtimes,
A balanced diet,
Exercise,
Stress reduction.
© 2024 Bennett, Coleman & Company Limited

