- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
- Web Stories

When Breast Cancer Comes Back - It Doesn't Mean The End!
A breast cancer diagnosis is life-altering. The ignored lump, the dismissed nipple changes, it’s only when the final diagnosis arrives that the gravity of it all sinks in. Well, good news is that with timely intervention, breast cancer can be treated and controlled. You fight through treatment, begin to heal, grow your hair back, regain your strength—and slowly, life starts to feel normal again. Now imagine being told it’s back. A relapse. It is of course a tough blow to take.
Recently, author and filmmaker Tahira Kashyap spoke up about her breast cancer relapse with strength and honesty, reminding us that she’s not alone in this fight. Many women face relapses, and it requires a lot of courage.
Dr. Sachin Trivedi, Director of Medical Oncology, HCG Hospitals Cancer Centre, Mumbai, explains, “Breast cancer can relapse locally, which means in the same breast or chest area, regionally (nearby lymph nodes), or distantly, which we call metastatic relapse where it spreads to other organs like the bones, liver, lungs, or brain.”
Dr. Hemkant Verma, Surgical Oncologist at Sharda Care Healthcity, adds that a relapse occurs when dormant cancer cells become active again. “It can be emotionally devastating, but with medical advancements, many relapsed cancers can still be managed effectively. Early detection and prompt action are our best tools.”
Local or regional relapses, especially those that occur after a few years, are most often treatable. Doctors say that the 5-year survival rate can still be as high as 60–80%, depending on individual cases. However, metastatic relapse (Stage IV) isn’t considered curable, but it is manageable. Many patients go on to live active lives for several years. What matters most is early detection, how aggressive the cancer is, where it has spread, and how well the body responds to treatment.
Minimising the risk of relapse
While treatment is key, there are lifestyle choices that can help reduce the risk of a recurrence like avoiding smoking, limiting alcohol intake, maintaining a healthy weight, following a balanced, antioxidant-rich diet and staying physically active.
Doctor warns that hormone replacement therapy should only be taken if it is medically advised.
"Staying in close contact with your oncology team is crucial. Regular follow-ups, checkups, and screenings play a vital role in catching any signs of recurrence early. Also, it’s important to address lingering side effects, whether it’s fatigue, menopause symptoms, bone loss, or lymphedema. Even something as simple as daily walks or gentle yoga can improve physical and mental health outcomes," adds Dr Sachin. Physical healing is only one part of the journey. Emotional and mental wellbeing matter just as much. Whether it’s therapy, support groups, mindfulness, journaling, or creative expression, it’s important to have an outlet and a support system.
Dr. Dinesh Pendharkar, Director, Sarvodaya Cancer Institute, adds that cancer relapse isn't a failure, it’s simply a new chapter. “Cancer is complex and can evolve over time, developing resistance to earlier treatments. Some cells may lie dormant and later reactivate. But today, we have many treatment options: chemotherapy, radiation, targeted therapies, immunotherapy, and even clinical trials.”
He reminds patients that science is advancing rapidly. “A relapse doesn’t mean the end. It’s just the beginning of a new strategy. With better tools, better treatments, and stronger support systems, this is a fight we can face with renewed hope. Think of it as a spiral, you have already climbed so far, and now you are rising to the next level.”

Credits: Canva
Healing Through Nature: The Role of Naturopathy In Modern Health Practices
As times are changing, all of us are going back to traditional approaches, whether it is Ayurveda, Homoeopathy or Naturopathy. These are alternative medicines and are useful in treating many diseases, especially through lifestyle changes. Most of these alternative medicines focus on preventive care. Today, we try to find out what one might be in for when they choose Naturopathy as a way of healing. What does it do? How does it differ from Ayurveda? How can it complement the regular day-to-day modern medicines?
For this, the Health and Me team spoke to Dr Prashanth Shetty, Principal at SDM College of Naturopathy and Yogic Science, Ujire.
What Is Naturopathy?
As the doctor explains, Naturopathy is a holistic approach to medicine that believes in the body’s innate ability to heal itself. It focuses on the root cause of illnesses, not just symptoms, and promotes natural healing through diet, lifestyle modifications, herbal remedies, hydrotherapy, and physical therapy.
"Naturopathy emphasizes natural healing, disease prevention, and lifestyle modification, aiming to restore balance and promote long-term wellness,” says Dr Shetty.
Unlike allopathic medicine, which often relies on pharmaceuticals and surgeries to treat disease symptoms, naturopathy works by supporting the body’s self-healing process.
How Does Naturopathy Complement Modern Medicine?
Naturopathy is increasingly being integrated with modern medical practices. It works well as a complementary therapy, especially in managing chronic conditions. For instance, naturopathic therapies such as acupuncture and nutrition counselling can reduce side effects of medications or improve treatment outcomes.
Patients undergoing treatment for diabetes, hypertension, arthritis, or even cancer may benefit from a combined approach—using conventional medications alongside naturopathic suggestions on diet, exercise, and stress reduction. This not only reduces dependency on medication but also empowers patients to actively participate in their healing journey.
Can It Help With Chronic Conditions?
Dr Shetty points out instances where Naturopathy has helped patients who have been battling with chronic diseases:
Diabetes: Naturopathic approaches like dietary changes, herbal supplements, and stress management can complement conventional treatments.
Hypertension: Lifestyle modifications, such as diet, exercise, and stress reduction, can be used alongside medication to manage blood pressure.
Arthritis: Naturopathic treatments like acupuncture, herbal remedies, and physical therapy can help manage pain and inflammation.
Mental Health
Anxiety and Depression: Naturopathic approaches like mindfulness, meditation, and herbal supplements can be used alongside conventional treatments.
Stress Management: Naturopathic techniques like yoga, deep breathing, and relaxation can help manage stress.
Digestive Health
Irritable Bowel Syndrome (IBS): Naturopathic approaches like dietary changes, probiotics, and stress management can help manage symptoms.
Inflammatory Bowel Disease (IBD): Naturopathic treatments like dietary modifications, herbal supplements, and stress reduction can complement conventional treatments.
Women's Health
Menstrual Disorders: Naturopathic approaches like herbal supplements, dietary changes, and stress management can help regulate menstrual cycles.
Menopause: Naturopathic treatments like herbal supplements, dietary changes, and lifestyle modifications can help manage symptoms.
Naturopathy vs Ayurveda: Are They the Same?
Though both systems promote natural healing, they are fundamentally different. “Naturopathy and Ayurveda are not the same—they are distinct systems of natural medicine with different foundations and limitations,” says Dr Shetty.
Naturopathy is grounded in the belief of self-healing through nature, whereas Ayurveda is rooted in the concept of balancing the body's three doshas—Vata, Pitta, and Kapha. Naturopathy commonly uses diet, hydrotherapy, and herbal medicines, while Ayurveda may include massages, herbal formulations, and treatments based on dosha types.
Additionally, naturopathic education is often structured and formalized, while Ayurvedic learning can also be passed down traditionally through apprenticeships.
While both the systems do share certain similarities—like emphasizing prevention, detoxification, and the use of herbal remedies; they follow a different framework and diagnostic methods. Naturopathy focuses more on individual's lifestyle and the environmental factors, whereas Ayurveda relies more on the ancient texts and doshic assessments, points out the doctor.
Personalized and Preventive
What makes naturopathy stand out is that it is personalized in nature and is based on each individual's lifestyle, their dietary habits, what suits them and what does not and their stress levels. It also evaluates emotional well-being, as well as the environment that may be the cause of their diseases or disorders.
At the core of naturopathy is prevention. It focuses more on preventing a disease even before the symptoms show up. By encouraging early lifestyle interventions, regular detoxification, and stress management, naturopathy helps reduce disease incidence, hospital visits, and the long-term burden on healthcare systems.
Reducing Healthcare Burden
There is an overgrowing burden on the healthcare system. While it is not to say that this must not be changed however, with alternative medicines like naturopathy, which emphasizes on preventive care, it can help lessen the burden. Naturopathy also focuses on educating individuals to take control of their health. The approaches used are: balanced nutrition, exercise, and mindfulness. As Dr Shetty notes, this not only empowers patients but also reduces the reliance on medication and minimizes hospital visits—ultimately easing the strain on healthcare infrastructure.
Credits: Canva
Young Non-Smoker Dies Of Terminal Lung Cancer After Being Misdiagnosed With Anxiety; Early Signs To Watch For
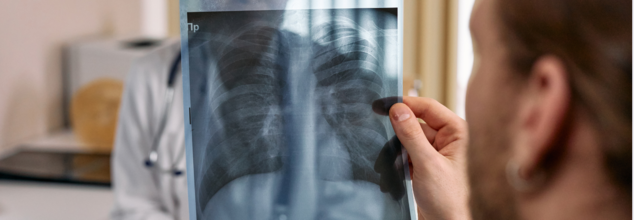
At 36-year-old Liam Handley, a fit, non-smoking man from Derbyshire, U.K., walked into his doctor’s office for the first time complaining of chest pain and palpitations, cancer was the last thing anyone suspected. Diagnosed instead with anxiety—a condition he had quietly battled for much of his adult life—Liam was sent home with increased doses of medication. What followed was a tragic and avoidable series of delays, assumptions, and overlooked warning signs that would eventually lead to his untimely death from terminal lung cancer.
Liam’s story is a heartbreaking reminder that lung cancer is not confined to those who smoke. It’s a wake-up call to patients, families, and healthcare professionals alike: lung cancer can strike anyone—regardless of lifestyle, age, or medical history.
Liam, who had red hair and dyslexia, often found himself subject to ridicule growing up. Later, his anxiety became a quiet undercurrent of his identity—something that doctors all too readily used as a blanket explanation for any new symptoms. When he reported persistent chest pain, shortness of breath, and palpitations, these signs were attributed to psychological stress.
His mother, Lynn Handley, still wonders how such critical symptoms could be missed. “Liam did not fit the stereotypical image of a lung cancer patient. He was young, a non-smoker, and in relatively good shape,” she said. “It wasn’t in our heads—and it clearly wasn’t in the GP’s either. And that’s the problem.”
How Early Signs Were Overlooked
When Liam’s symptoms intensified in mid-2020, his father took him to the hospital fearing a heart attack. Doctors discovered blood clots in his lungs—a red flag for a more serious underlying issue—but treated the clots with blood thinners and planned a CT scan that never happened due to COVID-19 delays.
As weeks passed, Liam's pain spread to his shoulders and lower back. He was prescribed stronger pain medication, but still, no further imaging or diagnostic testing was conducted by the public healthcare system. Eventually, the family paid out-of-pocket for a private CT scan. That scan changed everything.
Liam was diagnosed with metastatic lung adenocarcinoma, a form of non-small cell lung cancer that had already spread to his liver, spine, lymph nodes, and bones. The subtype—EGFR Exon19 positive—is a genetically driven mutation that disproportionately affects non-smokers and younger patients.
Despite being given just 5-6 weeks to live, Liam initially responded well to targeted therapy with Osimertinib, chemotherapy, and immunotherapy. He even married his long-term partner Louise in a quiet ceremony. For a brief moment, life seemed to regain some normalcy.
But by April 2021, the cancer had progressed. His treatments stopped working, and Liam’s health began to deteriorate rapidly. Dependent on oxygen, and weakened by disease, Liam passed away in October 2021—just shy of his 37th birthday.
Lynn Handley is now committed to raising awareness about lung cancer in people who don’t smoke. “We were angry. It took nine months for Liam to get a diagnosis. Those were months we could have used to fight harder, to plan better, to say goodbye on our own terms.”
Her advocacy isn’t just rooted in grief—it’s a call to action for healthcare systems and patients around the world.
Can Non-Smokers Get Lung Cancer?
Contrary to long-held assumptions, a significant proportion of lung cancer cases now occur in people with no history of smoking. The American Cancer Society reports that approximately 10-20% of lung cancers in the U.S. are found in non-smokers, often attributed to genetic mutations like EGFR, environmental exposures, or radon gas.
These cases are more common in women, younger adults, and individuals of East Asian descent, but—as Liam’s story demonstrates—they can affect anyone.
Early Signs and Symptoms to Look Out For
Lung cancer symptoms can mimic less serious conditions, which is why they’re often dismissed or misdiagnosed. If you experience the following symptoms persistently, don’t ignore them—regardless of your age or smoking history:
- Chest pain or discomfort
- Unexplained shortness of breath
- Persistent cough or wheezing
- Shoulder, back, or rib pain
- Fatigue or sudden weight loss
- Blood in sputum (though not always present)
Liam’s story is not just about a misdiagnosis—it’s about systemic bias. The assumption that lung cancer is a “smoker’s disease” delays diagnoses in healthy, younger adults. Primary care physicians and specialists must rethink their criteria for imaging and referrals. As Lynn Handley put it, “Why wasn’t a chest X-ray even considered?”
The COVID-19 pandemic added another barrier to care—delaying critical scans and overwhelming systems worldwide. But the cost of that delay, in Liam’s case, was irreversible.
If you're experiencing unexplained respiratory symptoms—don’t hesitate to ask for further investigation. Insist on imaging. Seek second opinions. Cancer doesn’t always follow the rulebook, and neither should your approach to protecting your health.

Credits: Canva
Headaches That Hurt Your Eyes: 5 Signs It’s Not Just Stress
Have you ever experienced one of those annoying headaches that's right behind your eyes, and it makes it even more difficult to concentrate or even keep your eyes open? You dismiss it, think of it as stress or getting too much screen time—but what if it's something more? Headaches related to eyes are a real thing, and they tend to go unnoticed until they begin affecting your daily activities. Whether you're always on your computer, missing eye exams, or simply believe it's "normal" to reach for a pain reliever and tough it out, this tale is your reminder to pause and pay attention to what your body—and even more specifically, your eyes—are trying to say.
Headaches are a common experience—unwelcome, usually inconvenient, and usually dismissed as the aftermath of a long day or hectic schedule but when that headache targets the back of your eyes and starts disrupting your daily routine, it's time to listen more intently. That is not tension alone it may be your body communicating something more.
For health professionals, especially ophthalmologists, chronic headaches that focus around or behind the eyes can be more than mere stress. They can be indicative of latent ocular or neurological conditions that require professional intervention. To learn when a headache can be more than just about stress—and when it's time to seek medical attention—we spoke with Dr. Neeraj Sanduja, an eye surgeon and ophthalmologist.
Link Between Your Headaches and Eyes
The eyes are intricate, high-performance organs which are used continuously—whether reading, driving, or working on computer screens. When they're being worked too hard or strained from underlying problems, they tend to express discomfort as headaches. These would usually be known as ocular headaches, and in contrast to those caused by stress, they can be accompanied with characteristic signs like eye pain, pressure, redness, or visual changes.
Dr Neeraj says, "The eyes are complex organs that work tirelessly throughout the day. When they are strained or affected by underlying conditions, the resulting discomfort can manifest as headaches. These headaches are often referred to as ocular headaches and can have specific characteristics that differentiate them from other types."
Curiously, pain felt in or around the eye isn't necessarily from the eye. Most of these are "referred pain"—a condition in which pain is felt in one location but is caused by another. This is why it is so easy to miss the actual cause, particularly when visual symptoms are minimal or none at all.
Signs Your Headache Isn't Just Stress
While stress is sure to produce headaches, the following indicators could mean that your headache stems from an eye condition or some other health problem:
1. Frequent or Daily Headaches Behind the Eyes
If you’re waking up with headaches or experiencing them routinely at the end of your workday, eye strain may be playing a central role. This is especially common in people with undiagnosed vision issues or those who stare at screens for extended hours.
2. Blurred or Fluctuating Vision
Headaches with associated changes in your ability to see clearly may point to issues like astigmatism or imbalance of the eye muscles. Such vision inconsistencies make the eyes work harder, resulting in pain that is referred to the temples or brow.
3. Eye Pain Without Redness or Obvious Irritation
If your eye appears to be fine but you still have pain in deep or rear parts of your eye, it might be connected to neurological or inflammatory disorders like optic neuritis. This necessitates urgent professional attention to eliminate pressure buildup or other severe conditions.
4. Glare, Halos, or Nausea
Conditions like glaucoma may raise intraocular pressure, leading to severe headaches and sensations like halos around lights, vomiting, or extreme eye pain. These are warning signs of the utmost concern that need immediate attention.
5. Difficulty with Focus and Coordination
A less familiar condition known as binocular vision dysfunction happens when the eyes are slightly out of alignment. This causes eye muscles to overwork, causing headaches, dizziness, and problems concentrating. Even slight misalignments can drastically affect your quality of life.
Dr Neeraj shares a list of causes which could indicate more than just a simple headache, indicating towards a serious problem at times.
Common Eye-Related Causes of Headaches
Eye Strain (Asthenopia): Prolonged activities like reading, using digital screens, or driving can strain the eye muscles. This strain often leads to a dull ache around the eyes or temples.
Uncorrected Vision Problems: Conditions such as nearsightedness (myopia), farsightedness (hyperopia), or astigmatism can cause the eyes to work harder to focus. This extra effort may result in headaches, especially after activities that require sustained focus.
Incorrect or Outdated Prescription Glasses: Wearing glasses or contact lenses with an incorrect prescription can strain the eyes, leading to headaches. Regular eye checkups are crucial to ensure your prescription is up to date.
Computer Vision Syndrome (Digital Eye Strain): Spending long hours in front of screens without adequate breaks can cause headaches due to digital eye strain. Symptoms may also include dry eyes, blurred vision, and neck pain.
Glaucoma: This condition increases intraocular pressure and can cause intense headaches, often around the eyes. Headaches due to glaucoma may be accompanied by symptoms like nausea, vomiting, or halos around lights.
Eye Muscle Imbalance: Misalignment of the eyes, even if minor, can lead to strain as the muscles work harder to maintain focus. This condition, known as binocular vision dysfunction, can cause frequent headaches.
Inflammatory Eye Conditions: Conditions like uveitis or optic neuritis (inflammation of the optic nerve) may cause severe headaches along with other symptoms such as vision changes or eye redness.
When to Seek Professional Help?
Dr Neeraj recommends, "If you experience headaches frequently and suspect they might be related to your eyes, it’s important to consult an ophthalmologist." If you’ve tried lifestyle adjustments, hydration, and stress management, and your headaches still persist, it’s time to look beyond the usual suspects. Consider seeking medical attention if:
- The headache is persistent or worsening.
- The headache is accompanied by blurry vision, eye pain, or redness.
- There are additional symptoms such as nausea, sensitivity to light, or difficulty focusing.
- You haven’t had a comprehensive eye examination in over a year.
Even if your symptoms appear to be under control, getting checked out early can avoid complications and reveal underlying conditions that could otherwise go undetected.
Diagnosis and Treatment for Eye-Related Headache
When you go to see an ophthalmologist for headaches, the test normally involves a complete determination of your visual acuity, intraocular pressure, and assessment of the optic nerves. Often, the issue might not be in the eye itself but how the eyes work together or how external usage such as screen time is affecting their health.
Depending on the diagnosis, your treatment could include:
- Corrected vision eyeglasses or contact lenses, updated.
- Lifestyle changes such as the 20-20-20 rule: look 20 feet away every 20 minutes for 20 seconds.
- Surgery or even medication for more severe conditions like glaucoma.
- Vision exercises or therapy for binocular vision dysfunction.
Prevention and Long-Term Eye Care
To avoid eye-related headaches, begin with routine eye exams—even if you don't wear glasses. When working extensively on computers or other digital devices, keep your work area well-lit, employ blue light filters, and take regular visual breaks. Drinking water and stress management will also contribute to overall eye and brain health.
It's also worth mentioning that kids and adolescents increasingly are also coming in with similar symptoms, particularly with our screen-dominated life. So, parents are to stay vigilant about behavioral signs such as irritability, squinting, or complaints of eye strain in younger generations.
All headaches are not equal. If yours center around or behind the eyes, or if they come with visual problems as a bonus, don't attribute them to stress without a probe. Your eyes may be sending a message your body can't ignore.
Dr Neeraj Sanduja is a MBBS, MS, Ophthalmologist, and Eye Surgeon at Viaan Eye and Retina Centre in India
© 2024 Bennett, Coleman & Company Limited

