- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
What Is Chikungunya And How Can It Be Prevented?

Chikungunya Disease and Prevention (Credits-Freepik)
Overview
This is a disease that is transmitted from mosquitoes to humans and affects many people in the world. Found in densely populated countries and continents, like Africa, Asia and the tropics of the Americas, this has severe symptoms. This viral disease is caused by the Chikungunya virus of the Togaviridae. First identified in the United Republic of Tanzania in 1952 and subsequently in other countries like Africa and Asia. Since 2004 the outbreak of CHIKV virus has become more widespread and caused partly due to the viral adaptations allowing the virus to be spread more easily by Aedes albopictus mosquitoes. The transmission has been noted to persist in countries where there is a large population, but interestingly, the transmission has been interrupted on islands where a high proportion of the population is infected and then immune.
Symptoms
The onset of the disease is usually in 4-8 days and after a bite of an infected mosquitoes, it is characterized by an abrupt onset of fever and then joint pain. This joint pain is severed and lasts for a few days but may prolong for months maybe even years. Other signs are joint swelling, muscle pains, headache, nausea, fatigue and rash. These symptoms also overlap with those of dengue and Zika virus and can be misdiagnosed. Most people fully recover from the infection and experience only mild and sometimes the infection even goes unrecognized. However, there have been cases of eye, heart, and neurological complications. The elderly and newborns are more susceptible to the infection and if they have any underlying conditions then they are likely to become severely ill increasing the risk of death.
Diagnosis and treatment
The diagnosis and treatment of the virus may be done by blood sampling and other tests like reverse transcriptase–polymerase chain reaction (RT–PCR). Other tests detect the activity of the antibodies. These can be detected in the first week after illness onset and can be detected for about 2 months. Many clinical measures can be taken to address fever and joint pain. But there is no specific anti-viral drug treatment for the virus.
Preventing Chikungunya
As this disease is caused by the bite of a mosquito, you must reduce the opportunities to let the mosquito breed. Mosquitoes bite during the day and night, and for people who live in risk areas like southeast Asia, Africa and tropical regions of America, many outbreaks happen each year. The best way to prevent it is to protect yourself from the mosquito's bite. You also must get vaccinated before travelling to any of these regions. Use insect repellent, and wear long-sleeved shirts and pants. You can also treat your clothes and gear with permethrin. As we all know, they tend to breed in humid places and places where they have access to water, so try to close the rooms that are air-conditioned with screens and windows. Use nets and mosquito repellents if you are sleeping outside. There are many different types of mosquito repellents like paper, liquid etc, and they are quite effective. If your job needs, you to be stationary for long hours or frequently go outside you must take the necessary precautions.
Bleeding Disorders In Women: Gynaecologist Lists The Causes
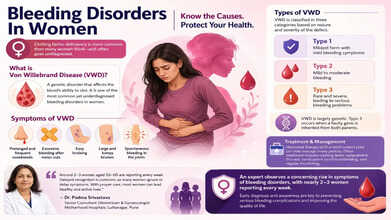
Early diagnosis and awareness are key to preventing serious bleeding complications and improving the quality of life. (Photo credit: AI generated)
Currently, there is a spike in cases of women being diagnosed with clotting factor deficiency, a condition where the blood does not clot properly. Many women aren’t aware of this and tend to dismiss it as routine menstrual concerns. While not always widely discussed, this condition can lead to serious health risks if not identified early. Hence, women should be more attentive and consult the doctor when they notice unusual bleeding patterns and improve their overall well-being.
What is Von Willebrand Disease?
One of the most common yet underdiagnosed conditions in women is von Willebrand disease. So, it is a genetic disorder that affects the blood’s ability to clot. Some women present as carriers of hemophilia or develop clotting issues due to liver disease, infections, hormonal imbalance, or nutritional deficiencies such as low vitamin K. Hence, women should pay utmost attention to their health.
What are the symptoms of VWD?
VWD is a common inherited bleeding disorder, and it occurs when there is a dysfunctional blood protein that does not let platelets clump together to form clots. Because it adversely affects the blood's ability to clot, it causes mucosal bleeding. In mild cases, the symptoms may not be there, but in other cases, the symptoms are the following:
- Prolonged and frequent nosebleeds
- Excessive bleeding after minor cuts
- Easy bruising
- Large and lumpy bruises
- Spontaneous bleeding in the joints
What are the types of VWD?
VWD is classified in three categories based on the nature and severity of the defect:
- Type 1: Mildest form with mild bleeding symptoms
- Type 2: Mild to moderate bleeding
- Type 3: Rare and severe, leading to serious bleeding problems
VWD is largely genetic, and the most extreme form—type 3—occurs when a faulty gene is inherited from both parents. For treatment, doctors recommend hormonal therapy like IUDs or birth control pills to manage heavy period bleeding.
“Clotting factor deficiency is seen when the body lacks certain proteins needed to stop bleeding. In women, this may be a genetic condition, such as hemophilia carriers or other inherited bleeding disorders. They can experience clotting factor deficiency because of liver problems, infections, hormonal imbalances, or nutritional deficiencies like low vitamin K levels. Women avoid the symptoms like bleeding gums, heavy period bleeding, and other issues, assuming that the symptoms with get better. However, prolonged bleeding is also reported by women, especially after gynaecological procedures like childbirth," Dr. Padma Srivastava, Senior Consultant Obstetrician & Gynaecologist, Motherhood Hospitals, Lullanagar, Pune, said in an interview with Health and Me.
Dr. Padma further added, “Around 2–3 women aged 50-60 are reporting every week. However, delayed recognition remains a major challenge, as many women tend to ignore symptoms or delay seeking medical advice. Management of this condition involves clotting factor replacement therapy, medications to control bleeding, and regular monitoring. With proper care, most women can lead healthy and active lives.”
Pregnancy After 35: Is It Prone To Complications?

Going for timely fertility evaluations is a good way to dodge the risk of pregnancy complications. (Photo credit: AI generated)
Changing lifestyles, career priorities, financial planning, and personal choices are leading many couples to marry later than before. While late marriages are becoming increasingly common, fertility specialists are observing a parallel rise in delayed pregnancy planning and age-related fertility complications. Many couples now begin trying to conceive only after the age of 35, when fertility in both men and women naturally starts declining.
Currently, there is a growing trend of late marriages due to career priorities, financial stability goals, higher education, and changing lifestyle choices. Many couples are choosing to settle professionally and personally before planning a family. However, this delay can also lead to postponed pregnancy planning, often at a stage when fertility naturally starts declining. Increasing stress, underlying medical conditions, and lack of fertility awareness are further contributing to challenges in conception among couples in their mid to late thirties.
What are the complications that can occur in a pregnancy after turning 35?
“The increasing trend of late marriages (30–35+) is directly leading to delayed pregnancy planning. Most couples start trying to conceive after 35, when fertility has already begun to decline significantly. By the time many patients seek medical help between 36 and 39 years, several are diagnosed with low ovarian reserve (low AMH) or conditions such as oligoasthenoteratozoospermia (OAT) and azoospermia.
Lack of early fertility awareness often causes women to miss the window for timely intervention or fertility preservation options like egg freezing. Advanced maternal age pregnancies (40+) are steadily rising and are often associated with complex complications and lower treatment success rates. Currently, nearly 75% of fertility patients are above 35 years of age, while 25% are above 40. Only around 20% of patients are in their late 20s,” said Dr. Jyotshana Palgamkar, Fertility Specialist, Nova IVF Fertility, Virar.
Dr Jyotshna further added, “One of the biggest concerns linked to late pregnancy planning is reduced ovarian reserve in women. By the time many women seek medical help between the ages of 36 and 39, their anti-Müllerian hormone (AMH) levels, which indicate egg reserve, may already be low. This reduces the chances of natural conception and can also affect the success rates of fertility treatments. Male fertility is also being affected. A large number of men are diagnosed with oligoasthenoteratozoospermia (OAT), a condition in which sperm count, motility, and morphology are affected.
Consequences of delayed fertility evaluation
Delayed fertility evaluation often means that couples lose valuable time before beginning treatment or considering assisted reproductive options. Another major challenge is the lack of awareness about fertility preservation. Many women remain unaware that egg freezing at a younger age may help preserve fertility for the future. By the time they start exploring fertility options in their late thirties or forties, treatment becomes more complex and emotionally stressful. Advanced maternal age pregnancies, especially above 40, are also increasing. These pregnancies are often associated with lower conception rates, higher miscarriage risk, pregnancy complications, and reduced IVF success rates,” Dr Jyotshna explained.
Male fertility treatment options depend on the underlying cause of infertility and may include lifestyle changes, medications, hormonal therapy, or surgical procedures. “Conditions such as low sperm count, poor sperm motility, abnormal morphology, raised DNA fragmentation index (DFI) affecting sperm quality, varicocele, or azoospermia can often be managed with timely medical intervention. Assisted reproductive techniques like IUI, IVF, and ICSI are also commonly used to improve the chances of conception. Early diagnosis and proper fertility evaluation play an important role in selecting the most effective treatment option for men,” said Dr Palgamkar.
Understanding fertility timelines, seeking timely evaluation, and discussing preservation options early can help couples make informed decisions and improve their chances of successful parenthood in the future.
Poor Posture, Disc Bulge: What Causes Back Pain In Young People
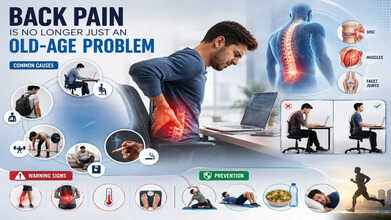
Lack of exercise can contribute to back pain. (Photo credit: AI generated)
Back pain is generally considered a problem seen in old age, but of late, we are increasingly seeing younger adults suffering from back pain. Prolonged sitting hours, inadequate physical activity, smoking, and an unhealthy lifestyle have made back pain a common complaint even in people under 30 years of age.
What is a slipped disc?
In an interview with Health and Me, Dr Pramod Sudarshan, Spine Surgeon (ortho), Apollo Hospitals, Bangalore, said, “Most commonly, we attribute this pain to a slipped disc or other disc-related conditions. However, they are just one among many reasons causing back pain. A thorough understanding of the other conditions that can lead to back pain, and knowing the ‘red flags’ to help identify them, will assist in seeking early treatment and preventing further complications.”
Muscle strain is considered to be one of the most common reasons for developing back pain in younger individuals. Daily activities like travelling for long hours, lifting heavy weights without proper technique, and carrying heavy backpacks can lead to muscle strain. Often, the pain due to muscle strain comes down with the help of medications such as muscle relaxants and rest.
Poor posture and back pain
Working professionals and students spend many hours a day studying, gaming, and working on computers without maintaining proper posture, leading to excess strain on the back muscles and, in turn, prolonged back pain. Having a properly ergonomically designed workstation/study table setup can prevent back discomfort and stiffness.
What are the causes of back pain?
Lack of physical activity and associated conditions such as obesity weaken our core muscles, which are considered the main pillars supporting our spine. Weakened core muscles will not be able to perform the functions expected of them, leading to back pain. Regular exercise, weight management, a healthy diet, and guided weight training will help strengthen our core muscles and reduce the risk of back pain.
Other than muscles, the spine also contains small joints known as facet joints, irritation or inflammation of which can lead to back pain. A structure known as the pars interarticularis acts as a clamp in the spine, holding two adjacent vertebral bodies, and any defect, such as a congenital defect or fracture due to repetitive microtrauma, as seen in gymnasts, can lead to the slipping of one bone over the other, causing back pain.
Though mechanical back pain is most common, there are other conditions such as inflammatory arthropathy, tumours, and infections. Conditions such as ankylosing spondylitis, rheumatoid arthritis, and hyperuricemia/gout are some examples of inflammatory conditions in which an individual experiences early morning back pain associated with stiffness and may also present with pain in other joints.
Can tuberculosis lead to back pain?
Tuberculosis affecting the spine is considered the most common infection of the spine. Severe back pain, weight loss, loss of appetite, fever, and night sweats are some of the common symptoms. Other bacterial and fungal infections are also seen affecting the spine, most commonly in immunocompromised individuals.
Tumours, though rare in young individuals, warrant further investigation when symptoms such as severe weight loss, night pain, and prolonged back pain are present to rule out the possibility of tumours.
Other conditions such as scoliosis (congenital/adolescent idiopathic scoliosis), which is a three-dimensional deformity of the spine, can cause back pain. It requires further assessment in the form of radiological investigations to assess the degree of deformity and to plan any surgical intervention, if required, based on the severity of the curve.
What are the symptoms?
Identifying some of the red-flag signs, such as weakness in the legs, numbness around the groin, bladder or bowel dysfunction, fever, unexplained significant weight loss, or severe pain following major trauma, is essential. These symptoms may indicate serious underlying pathology requiring medical care.
Fortunately, back pain in young people is largely preventable. Basic lifestyle modifications such as regular exercise, maintaining proper posture, avoiding prolonged sitting, maintaining a healthy body weight, undertaking monitored weight-training programmes, following a healthy diet, and getting adequate sleep will help prevent as well as overcome existing back problems. Invest in your spinal health at the earliest opportunity to reap the benefits in the second half of life.
© 2024 Bennett, Coleman & Company Limited

