- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
Spotting vs Period vs Bleeding: How To Identify
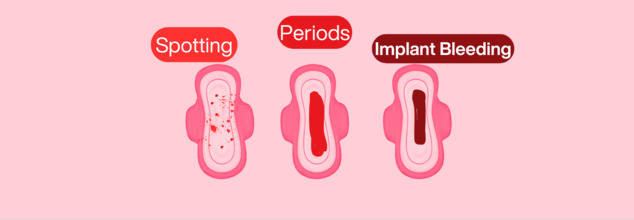
Image Credits: Health and me
A woman's health is intricately linked to her menstrual cycle, which is an important sign of her overall well-being. Throughout puberty and menopause, hormonal changes affect not only fertility but also mood, energy, and long-term health. A normal cycle usually indicates balance, whereas abnormalities may suggest problems such as PCOS, endometriosis, or thyroid disease.
Our bodies do not always work in a perfect clockwork operation and unexpected vaginal bleeding can often confused us. Is it a mere spotting? A normal period? A symptom of something more concerning? Differences between spotting, menstrual bleeding, and intermenstrual bleeding should be understood is crucial for maintaining reproduction health.
Here is a short guide to help you differentiate while you are confused.
Spotting
Spotting is vaginal bleeding that doesn't happen as part of your regular menstrual period. It commonly manifests as fine droplets or smears of blood on clothing or toilet tissue. The intensity of the blood ranges from deep red (recent blood) to pink (having cervical mucus mixed in it) or brown (older, oxidized blood). Spotting is not very much and can't be seen in a way that needs either a tampon or a pad to absorb.
Common Causes of Spotting
Spotting is caused by numerous factors, and in the majority of instances, it is nothing to worry about. Some frequent causes are:
Hormonal Birth Control Transitions: New birth control technique, for instance, birth control pills, IUDs containing hormones, or implants, results in temporary spotting as the body adapts.
Ovulation Bleeding: A few individuals get spotting light around the time of ovulation as a result of hormonal changes. It normally happens in the mid-cycle and could be followed by slight cramping.
Cervical Ectropion: A harmless condition when cells from the inside of the cervical canal migrate to the outer cervix, causing the outer cervix to become more sensitive and prone to faint bleeding on coitus or physical activity.
Early Pregnancy (Implantation Bleeding): 15–25% of pregnant women experience light spotting around 10–14 days post-conception, which is confused with an early period.
When to See a Doctor
Spotting is usually harmless, but it's best to consult a doctor if:
- It continues after a few months of initiating new birth control
- Is accompanied by pelvic pain or abnormal discharge
- Occurs after frequent intercourse
- Occurs during pregnancy and is not verified as implantation bleeding
Menstrual Bleeding
There is a time, also known as a period or menstruation, when the uterine lining sheds due to changing hormone levels. It would last for approximately 2-7 days and is heavier initially. The hue and texture of period blood shift during the menstrual cycle:
Red: New active bleeding at the start of a period
Brown or dark red: Older, slower blood in leaving the uterus
Clots: It's normal to have small clots, but bigger clots may be a sign of heavy menstrual bleeding (HMB)
Why You Have a Period Essentially?
Menstruation is a part of the reproductive cycle, and it happens around every 21–35 days. When there's no pregnancy after ovulation, hormone levels fall, causing the uterine lining to be shed.
Signs Your Period May Be Abnormal
Though periods differ in different people, there are some signs that point towards probable underlying conditions:
- Prolonged bleeding (longer than 7 days)
- Heavy flow necessitating pad/tampon changes every 1–2 hours
- Severe cramps that disrupt daily life
- Irregular periods or absent periods
If you have any of these, conditions such as polycystic ovary syndrome (PCOS), endometriosis, or thyroid disease may be involved, and a medical visit is in order.
Intermenstrual Bleeding
Unlike spotting, intermenstrual bleeding is heavier and unexpected between regular periods. It may be from bright red to dark brown and can contain blood clots.
Possible Causes of Bleeding Between Periods
Sexually Transmitted Infections (STIs): Chlamydia and gonorrhea can lead to inflammation and abnormal bleeding.
Pelvic Inflammatory Disease (PID): A bacterial infection of the reproductive organs and can lead to abnormal bleeding.
Uterine Fibroids or Polyps: Benign growths in the uterus that may cause unexpected bleeding.
Endometrial Hyperplasia or Cancer: In some instances, abnormal bleeding may be a sign of abnormal cell growth in the lining of the uterus.
When to See a Doctor
See a doctor if intermenstrual bleeding is:
- Frequent or persistent
- Associated with pelvic pain or discomfort
- Associated with abnormal discharge, fever or painful sex
Recognizing your body's rhythms can assist you in identifying normal versus abnormal bleeding. Monitoring your menstrual cycle through an app or calendar may flag changes that should be checked with a doctor. If you have any questions regarding abnormal bleeding, visiting your health care provider is the way to go.
Does Niacinamide Cause Purging? Dermatologist Insights

The most frustrating skincare experience is breaking out a week after using a new product. Niacinamide serum is the most common one that people blame when it happens. But the real question is: does Niacinamide cause purging? The answer is no, but understanding what happens in your skin when you introduce it can help you.
A well-formulated Niacinamide Serum at the right concentration is very gentle on the skin.
And pairing it with a Niacinamide Moisturizer helps your skin adjust if you are using it for the first time.
What Is Skin Purging and How Is It Different from Breakouts
Skin purging is the result of an active ingredient accelerating your skin's natural cell turnover cycle. Your skin renews itself every 28 days. Retinol, AHAs, and BHAs speed up this process, which pushes microcomedones, trapped sebum, and dead cell buildup up to the surface faster.
Your skin may appear like it is experiencing a sudden flare-up of pimples, but it is your skin clearing all the buildup in one go. True purging:
- Happens only with ingredients that increase cell turnover
- Appears in the same areas you normally break out
- Resolves within four to six weeks
- Involves small whiteheads and blackheads rather than deep cysts
A regular breakout appears in new areas with any product and does not follow the same predictable timeline. Understanding this difference is important before you blame any ingredient.
Does Niacinamide Cause Purging?
Dermatologists say no, and the reason comes down to how niacinamide works at the biological level. Purging occurs only when an ingredient accelerates cellular turnover, forcing the skin to shed faster to clear hidden congestion.
Niacinamide is a form of Vitamin B3, and its action is fundamentally different. It works in the following manner:
- Regulates sebum production through the sebaceous glands
- Strengthens the skin barrier by supporting ceramide production
- Niacinamide reduces redness and inflammation caused by acne
- Stops the transfer of melanin so that pigmentation reduces
Why Niacinamide Is Less Likely to Trigger Purging
No Cell Turnover Acceleration
Can niacinamide cause purging? Purging occurs when the old skin cells are shed, and new ones form at a faster pace. Niacinamide has no effect on this process. It works on controlling oil and improving barrier function. It does not work on exfoliation or renewal rate. There is no mechanism through which Niacinamide could cause purging without accelerating cell turnover.
Regulates Sebum, Doesn't Exfoliate
Niacinamide signals the sebaceous glands to produce less oil over time, whereas salicylic acid dissolves the sebum inside pores, and AHAs dissolve the bonds between dead skin cells. It reduces the congestion that leads to breakouts. Niacinamide for pimples works by calming the conditions that create them.
Reduces Inflammation Instead
The anti-inflammatory action of Niacinamide calms the redness and swelling around active breakouts. So, does niacinamide cause pimples? Its inflammation-reducing properties make it the safest active for acne-prone skin, which you can introduce at any concentration between 5% and 12%.
What Could Actually Be Causing Your Purging
If you started a niacinamide product and broke out, here are the more likely reasons for it.
New Product Adjustment
Any new skincare product can cause a temporary adjustment period as your skin gets used to a new formula or ingredients. This is not purging, but your skin reacting to change. It settles within one to two weeks if the formula is compatible with your skin.
Reaction to Other Formula Ingredients
Many niacinamide serums contain additional actives, such as AHAs, BHAs, Retinol, or exfoliating enzymes, which increase cell turnover in your skin. If your Niacinamide serum contains these ingredients as well, the purging may result from them. So, always check the full ingredient list before blaming a reaction on any single ingredient.
Wrong Concentration for Your Skin
Using a 20% Niacinamide formula directly when your skin has never used actives before can cause irritation that looks like a breakout. It's your skin reacting to a concentration that it is not ready for. A safe way is to start between 5% and 10% and build up slowly to prevent flare-ups.
How to Add Niacinamide Properly to Your Skincare Routine
The chances of a reaction reduce a lot when you introduce Niacinamide correctly.
1. Patch test first: Take a small amount and apply it to your inner arm or jawline, and observe for any reaction in the next 24 hours before using it on your full face. Gentle ingredients can react differently on certain skin types, so you must do a patch test.
2. Start at a lower concentration: 5% to 10% is the best starting point if you are a beginner. Give your skin four weeks at this level before going with anything stronger.
3. Introduce one product at a time: If you add multiple new products all at once, you will never know which one is causing a reaction. Add Niacinamide on its own first and give it two to three weeks before introducing other active ingredients.
4. Apply after washing your face: Niacinamide works best when the skin is fresh. Apply it after your face wash and before your moisturizer so that it absorbs better into the skin.
5. Be consistent: The oil-regulating and pore-refining benefits of Niacinamide show only after four to eight weeks of daily use. So, you may not get the results if you stop using it abruptly because of an unrelated reaction.
Conclusion
If you are still wondering, does niacinamide cause purging? It does not. An increase in cell turnover results in purging, and Niacinamide does not work that way. The main reasons for breakouts can be your skin trying to adjust to a new product or another active ingredient in the formula. Higher concentrations can also be tough for your skin to tolerate, which may result in breakouts.
Is Your BMI Score Reliable? Scientists Make A Shocking Revelation

A BMI score of 24 is considered normal. (Photo credit: AI generated)
Researchers have found that up to 25 per cent more adults could be classified as obese, even if their body mass index (BMI) score falls under the normal category. As per the current rules, a BMI score of 18.5 to 25 is considered healthy, 25–29 is overweight, and 30 onwards is considered obese. Obesity can contribute to a long-term risk of serious illness, but according to an international team of experts, BMI may not be the most reliable measure for ascertaining obesity levels in an individual.
Why is BMI not a reliable parameter?
Researchers have found that adding the weight-to-height ratio and waist circumference could be a good way to ascertain unhealthy body fat levels. Fat, according to scientists, builds up in people who are not considered overweight or obese under the current rules, depending on where it is stored. Older bodies have a higher fat build-up around the waist, which, when combined with loss of muscle mass, means that there is no change in total weight. This means that the fat that accumulates, known as "skinny fat," does not always raise an alarm.
The new study from scientists at the University of Southern California analysed data from 5,642 adults in the US and discovered that a quarter of them had a normal BMI but actually met the obesity criteria. Furthermore, over 50 per cent of overweight people, according to their BMI, also met the updated obesity criteria. These findings, according to experts, suggest that millions of Americans with obesity-related health complications could be missing much-needed health interventions.
BMI is problematic because it does not evaluate body fat but reflects total body weight, including muscle and bone. Therefore, a muscular person is likely to have a high BMI but not much fat. However, a person with a normal BMI can have excess body fat, which can lead to complications later. The good news, experts say, is that these obesity-related issues can be addressed. Either lifestyle changes, medication, or both can be effective in reducing body fat levels and lowering the risk of future health problems. The sooner it is diagnosed, the better it is for long-term well-being.
Read more: Why 'Normal Weight' Doesn’t Always Mean Healthy
Does obesity risk increase with age?
Researchers estimate that 30 per cent of adults living in England aged 16 years and above are obese. This increases with age, with over 35 per cent of people aged 55 to 74 years living with obesity. Under the new rules, obesity would be defined as a BMI of 30 and above, or at least one elevated measure, such as a high waist circumference, a high waist-to-height ratio, or a BMI of 40 and above. Researchers have labelled these obesity subtypes as BMI-plus-anthropometric obesity.
What is an unhealthy waist circumference?
According to the NHS, an unhealthy waist circumference is 37 inches in men and 31.5 inches or above in women. An unhealthy waist-to-height ratio occurs when the waist circumference is half or more of a person's height. According to the British Heart Foundation, BMI is calculated by dividing weight by height squared. There are multiple BMI calculators available online. It is classified as follows:
- Underweight – below 18.5
- Healthy weight – 18.5 to 24.9
- Overweight – 25 to 29.9
- Obese – 30 and above
If BMI is in the overweight category, it is linked with a heightened risk of heart disease and incidents such as stroke or heart attack. If it falls within the obese category, the risks are higher. Underweight people are not exempt from risk, as they have a greater likelihood of developing long-term health problems.
Can An App Be Your Therapist? India’s Digital Mental Health Revolution Faces Key Challenges

Credit: iStock
Millions of Indians are increasingly turning to mental health apps to manage stress, anxiety, loneliness, and other emotional challenges. These digital platforms offer a range of services, from mood tracking and mindfulness exercises to AI-powered chatbots designed to provide conversational support that can feel similar to therapy.
The growing adoption of such apps comes amid a significant shortage of mental health professionals in India. Data from the National Mental Health Survey indicate that nearly one in ten Indian adults lives with a diagnosable mental health disorder, while more than 85 percent of people with depression do not receive adequate treatment. Other studies have also highlighted a large gap between the demand for mental healthcare services and the availability of trained psychiatrists, psychologists, and counselors, particularly in rural and underserved regions.
Against this backdrop, mental health apps position themselves as a convenient and relatively affordable way to access support anytime and from anywhere. However, researchers and mental health experts caution that the rapid rise of these platforms has also sparked concerns about data privacy, the clinical effectiveness of digital interventions, and the level of oversight and accountability surrounding AI-driven mental health tools. While some studies suggest that digital mental health programs can help reduce symptoms of anxiety and depression, experts emphasize that they should complement—not replace—professional care, especially for individuals with moderate to severe mental health conditions.
Also Read: India's Maternal Mortality Ratio Drops From 130 To 87 In Last 10 Years: Govt
How Mental Disorders Are Impacting Life Worldwide?
Mental disorders are on the rise worldwide, and nearly 1.2 billion lives are now affected by them. A recent study published in The Lancet has revealed this very crucial trend. The study was conducted by researchers at the Institute for Health Metrics and Evaluation (IHME) in collaboration with the University of Queensland.
This study shows that the number of people affected by the mental disorder has almost doubled since 1990. It also emphasizes the role of mental disorder in the case of disability, as the research suggests that it has crossed cardiovascular disease, cancer, and musculoskeletal conditions, leading to disability. Notably, the study has revealed that mental disorders affect people of different sexes and ages disproportionately.
The research was done on a massive scale from 1990 to 2023. The researchers studied the impact of mental disorder on both sexes, in 25 age groups, 21 regions, and 204 countries and territories.
Over the years, mental disorders have caused more and more mayhem in people's lives. Disability adjusted life years (DALYs) show the very impact of mental disorders on life. DALYs measure the health loss. It calculates the years lived with disability and years of life lost due to premature death.
According to this very measuring system, we can see that the mental disorder and its impact on overall life reached another zenith in 2023. That year, mental disorders alone caused 171 million disability adjusted life years (DALYs). This made mental disorder the fifth biggest contributor to total disease burden. Notably, in 2023, mental disorders had a 17 percent share of total life lost due to disability throughout the world.
© 2024 Bennett, Coleman & Company Limited

