- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
Irregular Sleep, Drinking Caffeine After 3PM Could Raise Your Risk Of Heart Attack And Stroke

Irregular Sleep, Drinking Caffeine After 3PM Could Raise Your Risk Of Heart Attack And Stroke
I’ve always struggled with inconsistent sleep, staying up late and waking up at different times each day. My love for coffee was also on an all-time high with trying all the season specials. But it is only recently, I learned how this irregular sleep pattern and caffeine could increase my risk of heart attack and stroke. Now, I’m prioritizing a consistent sleep schedule and cutting out caffeine after 3 PM to protect my heart.
A new, shocking study shows that irregular sleep patterns can greatly increase the risk of heart attack and stroke. But that's not all: the timing of your caffeine intake could also play a critical role in your cardiovascular health. If you are struggling with inconsistent sleep patterns and regularly sipping on caffeinated beverages late in the day, you may be unknowingly putting yourself at risk for serious heart-related issues.
For most people, sleep is something of a given and we often only consider ourselves as long as we get our required seven to nine hours. However, according to a recent study conducted by researchers at the Children's Hospital of Eastern Ontario, it may not be that long after all. The study, which included more than 72,000 participants, found that people with irregular sleep patterns—those who fall asleep and wake up at vastly different times each day—face a 26% higher risk of experiencing a heart attack or stroke. This increased risk persisted even for those who managed to get enough sleep. The study followed up participants for eight years to track heart events such as heart attacks, strokes, and heart failure. The conclusions were clear: irregular sleep, even if it's sufficient in duration, is a major cardiovascular risk factor.
The researchers found that those whose sleep patterns were highly irregular had a significantly greater chance of life-threatening heart issues. The more erratic your sleep schedule, the greater the risk, regardless of how many hours you sleep. In fact, people with irregular sleep schedules showed worse cardiovascular health outcomes, including higher rates of high blood pressure, elevated stress hormones, and poor blood sugar and cholesterol management.
Senior scientist Dr. Jean-Philippe Chaput said "sleep regularity may be more relevant than sufficient sleep duration in modulating MACE [major adverse cardiovascular event] risk." In the study, it shows that our bodies are comfortable with consistency, and a varied sleep schedule may interfere with other processes that keep us healthy, especially the heart.
Is it Caffeine After 3 PM Causing Sleeplessness?
Another daily habit that may be putting your heart at risk is caffeine consumption after 3 PM. According to Dr. Chaput, the experts emphasize the need for a healthy sleep schedule and avoiding caffeine late in the day. Caffeine can stay in your blood for up to eight hours, and its consumption later in the afternoon can disrupt your sleep cycle.
Consistent, good-quality sleep is necessary for maintaining healthy cardiovascular function, and the disruption of this by late-day caffeine intake exacerbates the risks posed by irregular sleep. When you drink coffee, tea, or other caffeinated beverages too late, the stimulant effect on your nervous system makes it harder to fall asleep at a regular time. This can lead to inconsistent sleep patterns, which, as we have seen, can be harmful to heart health.
Dr Chaput insists that humans need to adopt practices that contribute to regularized sleep habits. This can be attained by establishing a proper sleeping and waking schedule, eliminating afternoon intake of stimulants such as caffeine, and making your body clock coincide with the lifestyle one leads.
How Does Poor Sleep Affect Heart Health?
According to the experts, the disturbance due to irregular sleep patterns impacts more than one physiological process involved in the maintenance of the healthy heart. For example, poor sleep can be associated with increased inflammation of the body, weakened immunity, and altered regulation of blood sugar and cholesterol, all of which contribute to increased blood pressure and weakening endothelial function, both associated with an increased risk for cardiovascular diseases. Sleep also plays a very important role in regulating stress hormones. Poor or disturbed sleep results in increased levels of cortisol, the stress hormone, which increases blood pressure and can have negative impacts on cardiovascular health over time.
Scientists hypothesize that these disturbances trigger a series of negative effects that enhance the risk of developing chronic heart conditions, including hypertension, atherosclerosis, or even heart failure.
Tips to Protect Your Heart and Improve Your Sleep
In order to protect your heart, experts recommend several proactive measures to improve your sleep patterns and lifestyle. First, maintain a regular sleep schedule whereby you go to bed and wake up at the same time every day, including weekends. Consistency will keep your body's internal clock in check.
Along with regulating your sleep, paying attention to your caffeine habits is just as important. To reduce your risk of heart disease and stroke, experts suggest avoiding caffeine after 3 PM. If you’re sensitive to caffeine, this rule becomes even more critical.
In addition, the introduction of stress-reducing activities like yoga or mindfulness can also be beneficial to lower cortisol levels, and therefore both sleep and heart health can improve. A diet rich in antioxidants, healthy fats, and low on processed sugars also helps maintain cholesterol levels and reduce inflammation.
Does Your Sleep Environment Also Has A Role To Play
Apart from the timing of caffeine and your sleep schedule, another very overlooked factor is the quality of your sleep environment. Scientists have long known that the environment in which you sleep has a huge impact on the quality of your rest. Poor quality of sleep, even if your sleep schedule is regular, can cause health risks that are very much the same as those that arise from irregular sleep patterns.
Here’s an additional tip: make sure your bedroom is conducive to restful sleep. This means keeping your room dark, quiet, and cool. A temperature of around 65°F (18°C) is ideal for most people. Consider investing in a comfortable mattress and pillows, and avoid screen time at least 30 minutes before bed to allow your brain to unwind.
Irregular sleep, in association with taking caffeine in late parts of the day, can risk heart attack and stroke, but a simple maintenance of a sleep schedule, the reduction of consumption of afternoon caffeine, and sleep environmental awareness can definitely safeguard one's heart along with total health.
Your sleep is more than just a time for rest; it's a vital component of your long-term health, and maintaining consistency in your sleep habits is one of the best things you can do for your heart.
Can An App Be Your Therapist? India’s Digital Mental Health Revolution Faces Key Challenges

Credit: iStock
Millions of Indians are increasingly turning to mental health apps to manage stress, anxiety, loneliness, and other emotional challenges. These digital platforms offer a range of services, from mood tracking and mindfulness exercises to AI-powered chatbots designed to provide conversational support that can feel similar to therapy.
The growing adoption of such apps comes amid a significant shortage of mental health professionals in India. Data from the National Mental Health Survey indicate that nearly one in ten Indian adults lives with a diagnosable mental health disorder, while more than 85 percent of people with depression do not receive adequate treatment. Other studies have also highlighted a large gap between the demand for mental healthcare services and the availability of trained psychiatrists, psychologists, and counselors, particularly in rural and underserved regions.
Against this backdrop, mental health apps position themselves as a convenient and relatively affordable way to access support anytime and from anywhere. However, researchers and mental health experts caution that the rapid rise of these platforms has also sparked concerns about data privacy, the clinical effectiveness of digital interventions, and the level of oversight and accountability surrounding AI-driven mental health tools. While some studies suggest that digital mental health programs can help reduce symptoms of anxiety and depression, experts emphasize that they should complement—not replace—professional care, especially for individuals with moderate to severe mental health conditions.
Also Read: India's Maternal Mortality Ratio Drops From 130 To 87 In Last 10 Years: Govt
How Mental Disorders Are Impacting Life Worldwide?
Mental disorders are on the rise worldwide, and nearly 1.2 billion lives are now affected by them. A recent study published in The Lancet has revealed this very crucial trend. The study was conducted by researchers at the Institute for Health Metrics and Evaluation (IHME) in collaboration with the University of Queensland.
This study shows that the number of people affected by the mental disorder has almost doubled since 1990. It also emphasizes the role of mental disorder in the case of disability, as the research suggests that it has crossed cardiovascular disease, cancer, and musculoskeletal conditions, leading to disability. Notably, the study has revealed that mental disorders affect people of different sexes and ages disproportionately.
The research was done on a massive scale from 1990 to 2023. The researchers studied the impact of mental disorder on both sexes, in 25 age groups, 21 regions, and 204 countries and territories.
Over the years, mental disorders have caused more and more mayhem in people's lives. Disability adjusted life years (DALYs) show the very impact of mental disorders on life. DALYs measure the health loss. It calculates the years lived with disability and years of life lost due to premature death.
According to this very measuring system, we can see that the mental disorder and its impact on overall life reached another zenith in 2023. That year, mental disorders alone caused 171 million disability adjusted life years (DALYs). This made mental disorder the fifth biggest contributor to total disease burden. Notably, in 2023, mental disorders had a 17 percent share of total life lost due to disability throughout the world.
Bleeding Disorders In Women: Gynaecologist Lists The Causes
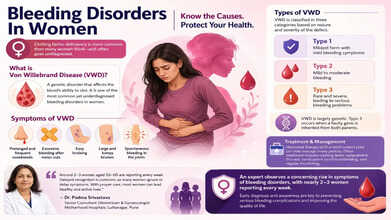
Early diagnosis and awareness are key to preventing serious bleeding complications and improving the quality of life. (Photo credit: AI generated)
Currently, there is a spike in cases of women being diagnosed with clotting factor deficiency, a condition where the blood does not clot properly. Many women aren’t aware of this and tend to dismiss it as routine menstrual concerns. While not always widely discussed, this condition can lead to serious health risks if not identified early. Hence, women should be more attentive and consult the doctor when they notice unusual bleeding patterns and improve their overall well-being.
What is Von Willebrand Disease?
One of the most common yet underdiagnosed conditions in women is von Willebrand disease. So, it is a genetic disorder that affects the blood’s ability to clot. Some women present as carriers of hemophilia or develop clotting issues due to liver disease, infections, hormonal imbalance, or nutritional deficiencies such as low vitamin K. Hence, women should pay utmost attention to their health.
What are the symptoms of VWD?
VWD is a common inherited bleeding disorder, and it occurs when there is a dysfunctional blood protein that does not let platelets clump together to form clots. Because it adversely affects the blood's ability to clot, it causes mucosal bleeding. In mild cases, the symptoms may not be there, but in other cases, the symptoms are the following:
- Prolonged and frequent nosebleeds
- Excessive bleeding after minor cuts
- Easy bruising
- Large and lumpy bruises
- Spontaneous bleeding in the joints
What are the types of VWD?
VWD is classified in three categories based on the nature and severity of the defect:
- Type 1: Mildest form with mild bleeding symptoms
- Type 2: Mild to moderate bleeding
- Type 3: Rare and severe, leading to serious bleeding problems
VWD is largely genetic, and the most extreme form—type 3—occurs when a faulty gene is inherited from both parents. For treatment, doctors recommend hormonal therapy like IUDs or birth control pills to manage heavy period bleeding.
“Clotting factor deficiency is seen when the body lacks certain proteins needed to stop bleeding. In women, this may be a genetic condition, such as hemophilia carriers or other inherited bleeding disorders. They can experience clotting factor deficiency because of liver problems, infections, hormonal imbalances, or nutritional deficiencies like low vitamin K levels. Women avoid the symptoms like bleeding gums, heavy period bleeding, and other issues, assuming that the symptoms with get better. However, prolonged bleeding is also reported by women, especially after gynaecological procedures like childbirth," Dr. Padma Srivastava, Senior Consultant Obstetrician & Gynaecologist, Motherhood Hospitals, Lullanagar, Pune, said in an interview with Health and Me.
Dr. Padma further added, “Around 2–3 women aged 50-60 are reporting every week. However, delayed recognition remains a major challenge, as many women tend to ignore symptoms or delay seeking medical advice. Management of this condition involves clotting factor replacement therapy, medications to control bleeding, and regular monitoring. With proper care, most women can lead healthy and active lives.”
Pregnancy After 35: Is It Prone To Complications?

Going for timely fertility evaluations is a good way to dodge the risk of pregnancy complications. (Photo credit: AI generated)
Changing lifestyles, career priorities, financial planning, and personal choices are leading many couples to marry later than before. While late marriages are becoming increasingly common, fertility specialists are observing a parallel rise in delayed pregnancy planning and age-related fertility complications. Many couples now begin trying to conceive only after the age of 35, when fertility in both men and women naturally starts declining.
Currently, there is a growing trend of late marriages due to career priorities, financial stability goals, higher education, and changing lifestyle choices. Many couples are choosing to settle professionally and personally before planning a family. However, this delay can also lead to postponed pregnancy planning, often at a stage when fertility naturally starts declining. Increasing stress, underlying medical conditions, and lack of fertility awareness are further contributing to challenges in conception among couples in their mid to late thirties.
What are the complications that can occur in a pregnancy after turning 35?
“The increasing trend of late marriages (30–35+) is directly leading to delayed pregnancy planning. Most couples start trying to conceive after 35, when fertility has already begun to decline significantly. By the time many patients seek medical help between 36 and 39 years, several are diagnosed with low ovarian reserve (low AMH) or conditions such as oligoasthenoteratozoospermia (OAT) and azoospermia.
Lack of early fertility awareness often causes women to miss the window for timely intervention or fertility preservation options like egg freezing. Advanced maternal age pregnancies (40+) are steadily rising and are often associated with complex complications and lower treatment success rates. Currently, nearly 75% of fertility patients are above 35 years of age, while 25% are above 40. Only around 20% of patients are in their late 20s,” said Dr. Jyotshana Palgamkar, Fertility Specialist, Nova IVF Fertility, Virar.
Dr Jyotshna further added, “One of the biggest concerns linked to late pregnancy planning is reduced ovarian reserve in women. By the time many women seek medical help between the ages of 36 and 39, their anti-Müllerian hormone (AMH) levels, which indicate egg reserve, may already be low. This reduces the chances of natural conception and can also affect the success rates of fertility treatments. Male fertility is also being affected. A large number of men are diagnosed with oligoasthenoteratozoospermia (OAT), a condition in which sperm count, motility, and morphology are affected.
Consequences of delayed fertility evaluation
Delayed fertility evaluation often means that couples lose valuable time before beginning treatment or considering assisted reproductive options. Another major challenge is the lack of awareness about fertility preservation. Many women remain unaware that egg freezing at a younger age may help preserve fertility for the future. By the time they start exploring fertility options in their late thirties or forties, treatment becomes more complex and emotionally stressful. Advanced maternal age pregnancies, especially above 40, are also increasing. These pregnancies are often associated with lower conception rates, higher miscarriage risk, pregnancy complications, and reduced IVF success rates,” Dr Jyotshna explained.
Male fertility treatment options depend on the underlying cause of infertility and may include lifestyle changes, medications, hormonal therapy, or surgical procedures. “Conditions such as low sperm count, poor sperm motility, abnormal morphology, raised DNA fragmentation index (DFI) affecting sperm quality, varicocele, or azoospermia can often be managed with timely medical intervention. Assisted reproductive techniques like IUI, IVF, and ICSI are also commonly used to improve the chances of conception. Early diagnosis and proper fertility evaluation play an important role in selecting the most effective treatment option for men,” said Dr Palgamkar.
Understanding fertility timelines, seeking timely evaluation, and discussing preservation options early can help couples make informed decisions and improve their chances of successful parenthood in the future.
© 2024 Bennett, Coleman & Company Limited

