- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
Fitness Tracking Apps May Be Fuelling Your Anxiety, Study Finds

(Credit-Canva)
With the extra busy schedules people have these days, fitness tracking apps have helped many people time and track their exercise time, calories burnt and the time taken to do so. These apps also remind us to drink water, not exceed our calorie limits for the day, as well as keep exercising. However, sometimes these devices can have an adverse impact on our health. Instead of making us feel better, they can make us feel anxious or stressed. This generally happens when we become too focused on the numbers and start to worry if they aren't perfect. It's important to understand that while these trackers can be helpful, they shouldn't control our mood or make us feel bad about ourselves.
A recent study published in the Journal of the American Heart Association also found that people with heart problems who used trackers were more worried about their symptoms. With so many people using these devices, it's becoming a common problem. 20% of wearable users felt anxious and always contacted their doctors when they received an irregular rhythm notification. They also found that these devices meant increased monitoring and worrying, higher usage of AFib (atrial fibrillation) specific health care etc. These findings suggest that while wearables can help patients monitor their AFib, they may also lead to increased anxiety and health care use. More research is needed to fully understand the effects of these devices on patients, doctors, and the health care system.
Signs These Apps May Be Getting Too Much For You
We can become too focused on achieving certain goals, like a certain number of steps or a perfect sleep score. This can lead to stress and anxiety when we don't meet those goals, instead of simply using the information to support a healthy lifestyle.
Your Metrics Influence Your Mood
If your happiness or sadness depends on the numbers your fitness tracker shows, it's a sign you might need a break. Getting a low score can make you feel like you've failed, even if you've been making healthy choices. It's normal to feel a little disappointed when you don't reach a goal, but your overall mood shouldn't be affected. If you notice that your mood changes a lot based on your tracker's data, it might be time to step away from it for a while.
You Constantly Try To Interpret Your Numbers
If you find yourself constantly searching online to understand what your tracker's data means, it's a warning sign. Trying to interpret every number can lead to more worry and confusion. You might start to believe you have health problems that don't exist. It's important to remember that these trackers are tools, not medical professionals. Spending too much time trying to decode the data can increase your anxiety instead of helping you.
You Feel Anxious When You Can’t See Your Data
If you feel nervous or anxious when you forget your tracker or it's not working, you might be too dependent on it. You should be able to feel comfortable and relaxed without constant data. If you feel panicky when you can't see your numbers, it's a sign you need to learn to be okay without them. You should be able to trust your body's signals instead of relying only on the tracker.
You’re Ignoring How Your Body Feels
If you rely only on your tracker and ignore what your body is telling you, it's a problem. Your body's signals are important. For example, you might feel well-rested, but if your tracker says your sleep quality is low, you might start to doubt yourself. It's important to listen to your body and not just the numbers. Your body knows when it's tired, hungry, or needs rest. The tracker is a tool to support your health, not replace your body’s signals.
Can An App Be Your Therapist? India’s Digital Mental Health Revolution Faces Key Challenges

Credit: iStock
Millions of Indians are increasingly turning to mental health apps to manage stress, anxiety, loneliness, and other emotional challenges. These digital platforms offer a range of services, from mood tracking and mindfulness exercises to AI-powered chatbots designed to provide conversational support that can feel similar to therapy.
The growing adoption of such apps comes amid a significant shortage of mental health professionals in India. Data from the National Mental Health Survey indicate that nearly one in ten Indian adults lives with a diagnosable mental health disorder, while more than 85 percent of people with depression do not receive adequate treatment. Other studies have also highlighted a large gap between the demand for mental healthcare services and the availability of trained psychiatrists, psychologists, and counselors, particularly in rural and underserved regions.
Against this backdrop, mental health apps position themselves as a convenient and relatively affordable way to access support anytime and from anywhere. However, researchers and mental health experts caution that the rapid rise of these platforms has also sparked concerns about data privacy, the clinical effectiveness of digital interventions, and the level of oversight and accountability surrounding AI-driven mental health tools. While some studies suggest that digital mental health programs can help reduce symptoms of anxiety and depression, experts emphasize that they should complement—not replace—professional care, especially for individuals with moderate to severe mental health conditions.
Also Read: India's Maternal Mortality Ratio Drops From 130 To 87 In Last 10 Years: Govt
How Mental Disorders Are Impacting Life Worldwide?
Mental disorders are on the rise worldwide, and nearly 1.2 billion lives are now affected by them. A recent study published in The Lancet has revealed this very crucial trend. The study was conducted by researchers at the Institute for Health Metrics and Evaluation (IHME) in collaboration with the University of Queensland.
This study shows that the number of people affected by the mental disorder has almost doubled since 1990. It also emphasizes the role of mental disorder in the case of disability, as the research suggests that it has crossed cardiovascular disease, cancer, and musculoskeletal conditions, leading to disability. Notably, the study has revealed that mental disorders affect people of different sexes and ages disproportionately.
The research was done on a massive scale from 1990 to 2023. The researchers studied the impact of mental disorder on both sexes, in 25 age groups, 21 regions, and 204 countries and territories.
Over the years, mental disorders have caused more and more mayhem in people's lives. Disability adjusted life years (DALYs) show the very impact of mental disorders on life. DALYs measure the health loss. It calculates the years lived with disability and years of life lost due to premature death.
According to this very measuring system, we can see that the mental disorder and its impact on overall life reached another zenith in 2023. That year, mental disorders alone caused 171 million disability adjusted life years (DALYs). This made mental disorder the fifth biggest contributor to total disease burden. Notably, in 2023, mental disorders had a 17 percent share of total life lost due to disability throughout the world.
Bleeding Disorders In Women: Gynaecologist Lists The Causes
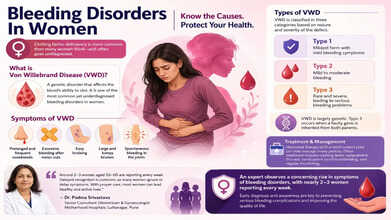
Early diagnosis and awareness are key to preventing serious bleeding complications and improving the quality of life. (Photo credit: AI generated)
Currently, there is a spike in cases of women being diagnosed with clotting factor deficiency, a condition where the blood does not clot properly. Many women aren’t aware of this and tend to dismiss it as routine menstrual concerns. While not always widely discussed, this condition can lead to serious health risks if not identified early. Hence, women should be more attentive and consult the doctor when they notice unusual bleeding patterns and improve their overall well-being.
What is Von Willebrand Disease?
One of the most common yet underdiagnosed conditions in women is von Willebrand disease. So, it is a genetic disorder that affects the blood’s ability to clot. Some women present as carriers of hemophilia or develop clotting issues due to liver disease, infections, hormonal imbalance, or nutritional deficiencies such as low vitamin K. Hence, women should pay utmost attention to their health.
What are the symptoms of VWD?
VWD is a common inherited bleeding disorder, and it occurs when there is a dysfunctional blood protein that does not let platelets clump together to form clots. Because it adversely affects the blood's ability to clot, it causes mucosal bleeding. In mild cases, the symptoms may not be there, but in other cases, the symptoms are the following:
- Prolonged and frequent nosebleeds
- Excessive bleeding after minor cuts
- Easy bruising
- Large and lumpy bruises
- Spontaneous bleeding in the joints
What are the types of VWD?
VWD is classified in three categories based on the nature and severity of the defect:
- Type 1: Mildest form with mild bleeding symptoms
- Type 2: Mild to moderate bleeding
- Type 3: Rare and severe, leading to serious bleeding problems
VWD is largely genetic, and the most extreme form—type 3—occurs when a faulty gene is inherited from both parents. For treatment, doctors recommend hormonal therapy like IUDs or birth control pills to manage heavy period bleeding.
“Clotting factor deficiency is seen when the body lacks certain proteins needed to stop bleeding. In women, this may be a genetic condition, such as hemophilia carriers or other inherited bleeding disorders. They can experience clotting factor deficiency because of liver problems, infections, hormonal imbalances, or nutritional deficiencies like low vitamin K levels. Women avoid the symptoms like bleeding gums, heavy period bleeding, and other issues, assuming that the symptoms with get better. However, prolonged bleeding is also reported by women, especially after gynaecological procedures like childbirth," Dr. Padma Srivastava, Senior Consultant Obstetrician & Gynaecologist, Motherhood Hospitals, Lullanagar, Pune, said in an interview with Health and Me.
Dr. Padma further added, “Around 2–3 women aged 50-60 are reporting every week. However, delayed recognition remains a major challenge, as many women tend to ignore symptoms or delay seeking medical advice. Management of this condition involves clotting factor replacement therapy, medications to control bleeding, and regular monitoring. With proper care, most women can lead healthy and active lives.”
Pregnancy After 35: Is It Prone To Complications?

Going for timely fertility evaluations is a good way to dodge the risk of pregnancy complications. (Photo credit: AI generated)
Changing lifestyles, career priorities, financial planning, and personal choices are leading many couples to marry later than before. While late marriages are becoming increasingly common, fertility specialists are observing a parallel rise in delayed pregnancy planning and age-related fertility complications. Many couples now begin trying to conceive only after the age of 35, when fertility in both men and women naturally starts declining.
Currently, there is a growing trend of late marriages due to career priorities, financial stability goals, higher education, and changing lifestyle choices. Many couples are choosing to settle professionally and personally before planning a family. However, this delay can also lead to postponed pregnancy planning, often at a stage when fertility naturally starts declining. Increasing stress, underlying medical conditions, and lack of fertility awareness are further contributing to challenges in conception among couples in their mid to late thirties.
What are the complications that can occur in a pregnancy after turning 35?
“The increasing trend of late marriages (30–35+) is directly leading to delayed pregnancy planning. Most couples start trying to conceive after 35, when fertility has already begun to decline significantly. By the time many patients seek medical help between 36 and 39 years, several are diagnosed with low ovarian reserve (low AMH) or conditions such as oligoasthenoteratozoospermia (OAT) and azoospermia.
Lack of early fertility awareness often causes women to miss the window for timely intervention or fertility preservation options like egg freezing. Advanced maternal age pregnancies (40+) are steadily rising and are often associated with complex complications and lower treatment success rates. Currently, nearly 75% of fertility patients are above 35 years of age, while 25% are above 40. Only around 20% of patients are in their late 20s,” said Dr. Jyotshana Palgamkar, Fertility Specialist, Nova IVF Fertility, Virar.
Dr Jyotshna further added, “One of the biggest concerns linked to late pregnancy planning is reduced ovarian reserve in women. By the time many women seek medical help between the ages of 36 and 39, their anti-Müllerian hormone (AMH) levels, which indicate egg reserve, may already be low. This reduces the chances of natural conception and can also affect the success rates of fertility treatments. Male fertility is also being affected. A large number of men are diagnosed with oligoasthenoteratozoospermia (OAT), a condition in which sperm count, motility, and morphology are affected.
Consequences of delayed fertility evaluation
Delayed fertility evaluation often means that couples lose valuable time before beginning treatment or considering assisted reproductive options. Another major challenge is the lack of awareness about fertility preservation. Many women remain unaware that egg freezing at a younger age may help preserve fertility for the future. By the time they start exploring fertility options in their late thirties or forties, treatment becomes more complex and emotionally stressful. Advanced maternal age pregnancies, especially above 40, are also increasing. These pregnancies are often associated with lower conception rates, higher miscarriage risk, pregnancy complications, and reduced IVF success rates,” Dr Jyotshna explained.
Male fertility treatment options depend on the underlying cause of infertility and may include lifestyle changes, medications, hormonal therapy, or surgical procedures. “Conditions such as low sperm count, poor sperm motility, abnormal morphology, raised DNA fragmentation index (DFI) affecting sperm quality, varicocele, or azoospermia can often be managed with timely medical intervention. Assisted reproductive techniques like IUI, IVF, and ICSI are also commonly used to improve the chances of conception. Early diagnosis and proper fertility evaluation play an important role in selecting the most effective treatment option for men,” said Dr Palgamkar.
Understanding fertility timelines, seeking timely evaluation, and discussing preservation options early can help couples make informed decisions and improve their chances of successful parenthood in the future.
© 2024 Bennett, Coleman & Company Limited

