- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
Daily Skincare Guide: Natural Remedies To Balance Oily And Acne-Prone Skin

Image Credit: Canva
The skin is an outward reflection of our internal health. Dull skin, for instance, may indicate dehydration, a lack of essential nutrients, or an inconsistent skincare routine. As the most visible organ, the skin also provides insight into the health of the body tissues it protects. It's more than just an aesthetic aspect—it’s a window into overall well-being. Disorders of the gut, blood, hormones, and even the heart can manifest as skin issues, such as rashes.
Ayurveda has long emphasized the importance of skincare. In today's fast-paced world, a proper skincare routine is indispensable, not only for physical health but also for mental well-being. While modern skincare offers a plethora of products, many come with side effects. Ayurveda provides a holistic solution, addressing skincare concerns naturally and sustainably.
Ayurvedic Skin Types
Ayurveda classifies skin types based on the three doshas:
1. Vata (Wind) Vata
Vatadominant individuals tend to have dry, rough skin that wrinkles easily if not properly moisturized.
- Oil application: Pinda taila is ideal for moisturizing dry skin.
- Internal care: Mahatiktaka ghrita helps reduce dryness.
- Face pack: Use Eladi churna or Navara rice face packs to moisturize and reduce dryness.
- Hydration: Drink plenty of water to combat dehydration.
2. Pitta (Fire) Pitta
Pitta dominant individuals often have oily skin, prone to acne, rosacea, and discoloration.
- Oil application: Nalpamaradi tailam is best for pitta skin.
- Cleansing: Wash your face with Eladi or Manjishtadi water to reduce discoloration and tone the skin.
- Cooling elements: Use aloe vera, turmeric, and sandalwood to combat inflammation, pimples, and redness.
3. Kapha (Water and Earth)
Kapha skin tends to be cold, oily, and prone to pimples, whiteheads, and water retention.
- Avoid oil-based creams: Use face masks regularly to control sebum production.
- Therapy: Dhara with Triphala churna or Eladi water is beneficial.
- Oil application: Eladi coconut oil is ideal.
Panchakarma for Healthy, Radiant Skin
Panchakarma therapies help detoxify the body and enhance skin health. Key treatments include:
Abhyanga and Pizhichil: These therapies pacify doshas, enhance skin tone, and act as natural moisturizers.
Navara Kizhi: Improves skin softness and complexion.
Snehapana: Internal lubrication with ghee to maintain hydration and promote a natural glow.
Ubtan: A traditional herbal paste for exfoliation and nourishment.
Lepam: Herbal poultices to soothe inflammation and heal skin conditions.
Garshan/Udwarthanam: Dry brushing to stimulate circulation and exfoliate dead cells.
Shirodhara: Oil pouring therapy to relax, de-stress, and improve sleep quality.
Panchakarma Detox: A five-step detoxification process to cleanse the body and rejuvenate the skin.
Internal Routine for Healthy Skin
1. Stay hydrated and drink 2–3 liters of water daily. Incorporate water-rich fruits and vegetables like watermelon, cucumber, and oranges. Herbal teas with ginger, lemon, or chamomile aid digestion and promote glowing skin.
2. Follow a balanced diet based on your Ayurvedic prakriti and elevated doshas. Include whole grains, dairy, seasonal fruits, and antioxidant-rich foods like tomatoes, broccoli, and papaya. Avoid fried, refined, and processed foods, as well as excessive sugar, salt, and red meat.
3. Regular exercise promotes blood circulation, detoxification, and skin nourishment. Activities like yoga, walking, or dancing improve oxygen flow, flushing out toxins and revitalizing the skin.
4. Maintain a consistent sleep schedule. Restful sleep stimulates growth hormones, promoting collagen and elastin production, which keeps skin firm and youthful.
Small, gradual adjustments in daily routines can lead to healthier, more radiant skin. Embrace an Ayurvedic skincare regimen, complemented by panchakarma therapies, to achieve sustainable and natural skin health.
Poor Posture, Disc Bulge: What Causes Back Pain In Young People
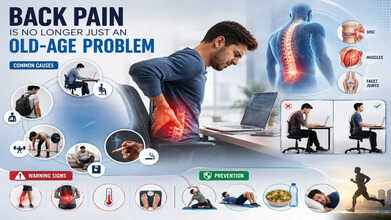
Lack of exercise can contribute to back pain. (Photo credit: AI generated)
Back pain is generally considered a problem seen in old age, but of late, we are increasingly seeing younger adults suffering from back pain. Prolonged sitting hours, inadequate physical activity, smoking, and an unhealthy lifestyle have made back pain a common complaint even in people under 30 years of age.
What is a slipped disc?
In an interview with Health and Me, Dr Pramod Sudarshan, Spine Surgeon (ortho), Apollo Hospitals, Bangalore, said, “Most commonly, we attribute this pain to a slipped disc or other disc-related conditions. However, they are just one among many reasons causing back pain. A thorough understanding of the other conditions that can lead to back pain, and knowing the ‘red flags’ to help identify them, will assist in seeking early treatment and preventing further complications.”
Muscle strain is considered to be one of the most common reasons for developing back pain in younger individuals. Daily activities like travelling for long hours, lifting heavy weights without proper technique, and carrying heavy backpacks can lead to muscle strain. Often, the pain due to muscle strain comes down with the help of medications such as muscle relaxants and rest.
Poor posture and back pain
Working professionals and students spend many hours a day studying, gaming, and working on computers without maintaining proper posture, leading to excess strain on the back muscles and, in turn, prolonged back pain. Having a properly ergonomically designed workstation/study table setup can prevent back discomfort and stiffness.
What are the causes of back pain?
Lack of physical activity and associated conditions such as obesity weaken our core muscles, which are considered the main pillars supporting our spine. Weakened core muscles will not be able to perform the functions expected of them, leading to back pain. Regular exercise, weight management, a healthy diet, and guided weight training will help strengthen our core muscles and reduce the risk of back pain.
Other than muscles, the spine also contains small joints known as facet joints, irritation or inflammation of which can lead to back pain. A structure known as the pars interarticularis acts as a clamp in the spine, holding two adjacent vertebral bodies, and any defect, such as a congenital defect or fracture due to repetitive microtrauma, as seen in gymnasts, can lead to the slipping of one bone over the other, causing back pain.
Though mechanical back pain is most common, there are other conditions such as inflammatory arthropathy, tumours, and infections. Conditions such as ankylosing spondylitis, rheumatoid arthritis, and hyperuricemia/gout are some examples of inflammatory conditions in which an individual experiences early morning back pain associated with stiffness and may also present with pain in other joints.
Can tuberculosis lead to back pain?
Tuberculosis affecting the spine is considered the most common infection of the spine. Severe back pain, weight loss, loss of appetite, fever, and night sweats are some of the common symptoms. Other bacterial and fungal infections are also seen affecting the spine, most commonly in immunocompromised individuals.
Tumours, though rare in young individuals, warrant further investigation when symptoms such as severe weight loss, night pain, and prolonged back pain are present to rule out the possibility of tumours.
Other conditions such as scoliosis (congenital/adolescent idiopathic scoliosis), which is a three-dimensional deformity of the spine, can cause back pain. It requires further assessment in the form of radiological investigations to assess the degree of deformity and to plan any surgical intervention, if required, based on the severity of the curve.
What are the symptoms?
Identifying some of the red-flag signs, such as weakness in the legs, numbness around the groin, bladder or bowel dysfunction, fever, unexplained significant weight loss, or severe pain following major trauma, is essential. These symptoms may indicate serious underlying pathology requiring medical care.
Fortunately, back pain in young people is largely preventable. Basic lifestyle modifications such as regular exercise, maintaining proper posture, avoiding prolonged sitting, maintaining a healthy body weight, undertaking monitored weight-training programmes, following a healthy diet, and getting adequate sleep will help prevent as well as overcome existing back problems. Invest in your spinal health at the earliest opportunity to reap the benefits in the second half of life.
New Vaccine May Prevent Bowel And Ovarian Cancer, Offering Hope for Millions
Credits: Canva
Researchers from the University of Oxford and pharmaceutical firm Moderna have developed a vaccine that may prevent bowel and ovarian cancer. The first trial is to be this summer, and it will try to see if the vaccine can train the immune system to recognize and eliminate pre-cancerous cells in people with Lynch syndrome before cancer develops.
In the United Kingdom, one in 300 people has Lynch syndrome, an inherited health condition that massively increases the chance of contracting cancers like bowel and ovarian cancer.
What Is Colorectal Cancer?
Colorectal cancer is the umbrella term for both colon and rectal cancer. As the name also suggests, colon cancers happen only in the colon, but if it is left untreated, it can spread to different organs in your body. Colorectal cancer begins inside the rectal tissues or the colon walls. It presents itself in the earliest stages as small masses, known as polyps. If a polyp becomes cancerous, it can spread cancer from the inner part of the colon to the lymph nodes or bloodstream. If this happens, cancer can then quickly move throughout the system.
Early Symptoms Of Colorectal Cancer
- Persistent changes in bowel habits, especially if they last more than a few days, must be taken seriously. Narrow or ribbon-shaped stools may indicate a tumor partially blocking the colon.
- Blood in the stool is one of the most common and concerning signs. While it might be due to hemorrhoids or fissures, it’s important not to assume. A proper evaluation is critical.
- Unexplained weight loss: Especially when unintentional.
- Abdominal cramps or bloating: Misinterpreted as common digestive issues.
What Is Ovarian Cancer?
Ovarian cancer is one of the deadliest gynecological cancers and is often referred to as the “silent killer” because its early symptoms are vague and easily mistaken for common digestive or urinary issues.
It develops when abnormal cells in the ovaries grow uncontrollably and may spread to other parts of the body. Survival rates are significantly higher when detected early—around 93 per cent of women diagnosed at stage one survive at least five years, compared to just 13 per cent at stage four, according to the American Cancer Society.
Unfortunately, many cases are diagnosed at advanced stages, when treatment options are limited, and outcomes are poorer.
- Early Symptoms Often Overlooked
“Ovarian cancer is commonly called a ‘silent disease’ because its early signs are vague and often resemble routine gastric issues,” Dr. Tejinder Kataria, Chairperson – Radiation Oncology, Medanta Hospital, Gurugram, told HealthandMe.
Common symptoms include:
- Persistent bloating
- Feeling full quickly or reduced appetite
- Pelvic or abdominal discomfort
- Unexplained constipation or diarrhea
- Ongoing indigestion
- Excessive gas
- Abdominal heaviness
Dr. Parminder Kaur, Consultant Gynaecologic Oncologist at CK Birla Hospital, Delhi, told HealthandMe that the key concern is when symptoms become frequent, persistent, and unusual for an individual’s normal health pattern.
Confused By Your Cholesterol Report? Here's What LDL And ApoB Really Mean

Credit: AI generated image
Every year, millions of people undergo routine health check-ups that include a lipid profile. Yet for many, the numbers on the report—Low-Density Lipoprotein (LDL), High-Density Lipoprotein (HDL), triglycerides, and increasingly ApoB—remain confusing.
Most people know that cholesterol is linked to heart disease and that "good" cholesterol can be beneficial, while high levels of "bad" cholesterol may increase cardiovascular risk. However, understanding what the different lipid profile numbers mean—and which ones matter most—can make a significant difference to long-term heart health.
Taking to the social media platform X, noted neurologist Dr. Sudhir Kumar said, "This is mainly meant for people who have NOT suffered a heart attack or stroke and are NOT already taking statins."
How Often Should You Get Tested?
Dr. Sudhir, Senior Consultant Neurologist at the Institute of Neurosciences, Apollo Hospitals, Hyderabad, shared that for most healthy adults, a lipid profile every two to three years is generally sufficient.
However, more frequent testing may be necessary for people with:
- Diabetes
- High blood pressure
- Obesity
- A history of smoking
- A family history of premature heart disease
- Previously abnormal cholesterol levels
LDL: Why This Cholesterol Matters
Also read: AHA’s New Dyslipidemia Guidelines Stress Early Screening, Lifestyle Management
LDL cholesterol, commonly known as LDL-C, is often referred to as "bad cholesterol." The expert explained its key role in the development of heart disease.
"Excess LDL can enter artery walls and contribute to plaque formation. Over time, these plaques may narrow blood vessels or rupture, increasing the risk of heart attacks and strokes," Dr. Sudhir said.
For most healthy adults, LDL levels below 100 mg/dL are considered desirable. Levels above this range gradually increase cardiovascular risk, particularly when elevated over many years.
The lower the LDL, the lower the long-term risk of heart attack and stroke. On the other hand, persistently high LDL can increase the lifetime risk of:
- Heart attack
- Stroke
- Peripheral artery disease
Triglycerides: A Marker Of Metabolic Health
Triglycerides are another type of fat found in the bloodstream. High levels of triglycerides are often a marker of poor metabolic health, Dr. Sudhir said.
He added that high triglycerides can indicate:
- Insulin resistance
- Obesity
- Prediabetes
- Diabetes
- Physical inactivity
- Excessive alcohol consumption
- Diets rich in refined carbohydrates and sugary beverages
What About HDL?
High-density lipoprotein, or HDL, has long been known as "good cholesterol." Traditionally, higher HDL levels have been associated with lower cardiovascular risk.
However, recent research has challenged the idea that simply raising HDL improves heart health. Several medications designed to increase HDL levels failed to reduce heart attack risk, prompting a shift in focus toward lowering harmful cholesterol particles rather than boosting HDL alone.
As a result, the expert cautioned against judging cardiovascular health based solely on HDL levels.
ApoB: The Emerging Risk Marker
Read More: Cardiovascular Diseases Lead As India’s Top Killer: US Cardiologist Points Out Risk Factors
One of the most important developments in cardiovascular prevention is the growing recognition of Apolipoprotein B, or ApoB. Dr. Sudhir stated that ApoB is a protein found on potentially harmful cholesterol-carrying particles such as LDL and VLDL (Very Low-Density Lipoprotein, a type of "bad" cholesterol).
"Think of ApoB as a count of the particles capable of entering artery walls and causing plaque. One ApoB is equal to one potentially harmful particle," the expert said.
ApoB is important because two people may have the same LDL level, but only one may have many more cholesterol-carrying particles. That person will often have a higher ApoB level and potentially higher cardiovascular risk. ApoB often provides a more accurate assessment of risk than LDL alone, the neurologist explained.
He suggested that ApoB testing should be considered by people with diabetes, prediabetes, metabolic syndrome, obesity, elevated triglycerides, or a strong family history of heart disease.
How To Improve Lipid Profile Naturally?
Dr Sudhir said that one should focus on long-term cardiovascular health, and not just a single laboratory number. He added that one can improve their lipid profile and thereby heart health by:- Exercising regularly
- Maintaining a healthy body weight
- Avoiding smoking
- Limiting sugary drinks
- Reducing ultra-processed foods
- Eating more vegetables, fruits, and legumes
- Choosing healthier sources of fat
- Prioritizing good sleep.
© 2024 Bennett, Coleman & Company Limited

