- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
Woman Left Screaming In Pain After Sex Toy 'Pulled Through Body' During MRI Scan
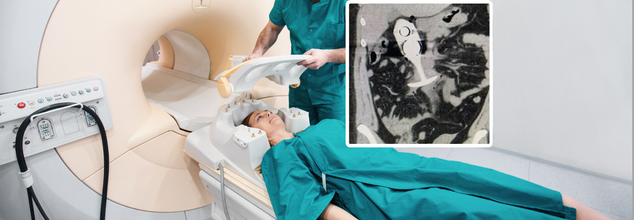
MRI scans are strong diagnostics with high-definition images of what lies inside a body. Strong magnetic fields require precaution, as brought out by an instance where a young woman suffered very serious injuries due to an oversight in a metallic core within a silicone sex toy that she happened to have before the MRI scan. This makes a stark reminder about the potentially deadly consequences of missing metal objects when such procedures are being performed. In April 2023, a 23-year-old woman went into an MRI with a silicone plug containing a metal core that was not known.
She thought that the item is made entirely out of silicone according to the advertising. However, the strong magnetic field of the MRI machine interacted with the hidden metal, dragging the object through her body and causing excruciating pain. According to reports from the U.S. Food and Drug Administration (FDA), the scene was harrowing, with the woman screaming in agony and requiring immediate hospitalization. Despite pre-scan screenings, which are routine prior to a scan, the patient did not inform the facility that the object existed because he presumed it was purely non-metallic. This caused serious injuries that led to the patient's law suit against the manufacturer for deceitful misrepresentations of material content.
MRI machines employ magnets between 0.5 to 3 Tesla (T). This is thousands of times stronger than the Earth's magnetic field. The tremendous force causes ferromagnetic materials, like iron and nickel, to be magnetized quickly and become strongly attracted toward the magnet. Objects as small as hairpins or paper clips will accelerate at 40 miles per hour inside the magnetic field.
The force can lead to catastrophic injuries in items lodged within the body, such as metallic implants or foreign objects. Metallic cores within devices, like pacemakers or intrauterine devices, must be disclosed to radiologists to prevent such complications.
How Metal Objects Interact with MRI Fields?
On these claims, Dr. Adam Taylor, a specialist in human anatomy, weighed his words in a international health website and added that the distance away and mass of this object would increase its velocity towards that of sound, "The acceleration would be phenomenal, but with a metallic core, it can't go anywhere near supersonic speeds. As for the size, the magnetic acceleration to the internal soft tissues would ensure that there could be severe intracranial trauma."
The injuries inflicted in this case likely involved damage to major blood vessels, nerves, or organs, highlighting the devastating impact of even minor oversight during an MRI scan.
This is not an isolated case. There are documented cases of metallic objects causing serious damage during MRI scans with a 65-year-old man with schizophrenia swallowed metal objects, including sockets and a hinge pin. The powerful magnetic field during an MRI scan caused the objects to rupture his stomach, resulting in serious injuries.
A toddler who ingested 11 small magnets perforated his bowel while undergoing a scan, making his case unique. In another deadly but extremely rare incident, there have been people who hide a firearm on themselves during MRI procedures. Magnetic attraction can trigger a discharge in a weapon and has led to some fatal injuries.
These cases emphasize the very strong need for adequate screening and patient education prior to an MRI.
Preventing MRI-Related Incidents
Medical professionals have been trained to avoid risks. This is by properly screening a patient for metallic objects. In general, most pre-scan protocols include:
- Patients are interrogated about implants, recent surgery or exposures at work related to metals.
- Radiologists sometimes use handheld metal detectors to search for hidden items.
- People who work with metal, like welders or machinists, will need additional testing to detect microscopic metal fragments within soft tissues or eyes.
The case emphasizes the importance of product labeling by manufacturers, especially those products that are likely to unintentionally cause harm to health. The patient's assumption that her device was 100% silicone points to a larger problem in consumer markets with misinformation.
It also reminds the patients to report any possible dangers to the medical professionals, no matter how the objects look non-metallic. In sensitive cases, patients can request private discussions with healthcare providers to ensure safety without discomfort.
In the end, it is a joint effort from manufacturers, healthcare professionals, and patients that can prevent such tragedies. Manufacturers must ensure truthful marketing, while healthcare providers should educate patients about the dangers of metal objects in MRI settings. For patients, understanding the risks and actively participating in pre-scan disclosures can be lifesaving.
This young woman's experience is a sobering example of the unforeseen dangers posed by MRI machines when precautions are overlooked. It serves as a wake-up call to address gaps in patient awareness, medical protocols, and product transparency. By learning from this incident, the medical community and the public can work together to ensure MRI scans remain a safe and effective diagnostic tool.
Alcohol Study Shelved By Trump Administration Published In Scientific Journal: What Did It Find?

Credit: Canva
A federally commissioned study that concluded even low levels of alcohol consumption may increase the risk of disease and premature death has now been published in a scientific journal after its findings were set aside by the Trump administration.
The study, known as the Alcohol Intake and Health Study, was commissioned as part of an effort to update the United States Dietary Guidelines. Researchers concluded that consuming as little as one alcoholic drink per day could raise the risk of serious illness and mortality.
However, the report was never officially released by the administration and later became the subject of political and industry scrutiny.
Why Was the Study Not Released?
Launched in 2023, the Alcohol Intake and Health Study was overseen by the Substance Abuse and Mental Health Services Administration (SAMHSA).
The review aimed to inform recommendations on alcohol consumption in the next edition of the federal dietary guidelines. But soon the study garnered controversy with some members of Congress and alcohol lobby groups arguing that scientists involved in the review held anti-alcohol views, according to Stat News.
As per a House Oversight Committee report, released in January, the study was "irretrievably flawed". It recommended that federal officials disregard its findings when drafting dietary guidance.
However, researchers involved in the project argued that the findings were sidelined because they conflicted with the interests of the alcohol industry.
What Did The Study Find?
Also read: Is There A Safe Limit For Alcohol Consumption? Major Review Challenges Long-Held Beliefs
After the federal review was shelved, researchers submitted their work independently to the Journal of Studies on Alcohol and Drugs, where it was published following peer review.
The published analysis concluded that even modest alcohol consumption — roughly one drink per day — is associated with increased risks of disease and death.
“These findings are not radical. They are rigorous — and commercially threatening,” wrote Robert Vincent, a former SAMHSA associate administrator for alcohol prevention and treatment policy, in an accompanying editorial.
Vincent, who helped oversee the project, lost his position during broader cuts across federal health agencies last year, the report said.
Notable, the US Department of Health and Human Services (HHS) has stated that the now published article was not the same report reviewed by the government and emphasized that it was not commissioned, approved, or cleared by SAMHSA.
Alcohol Guidance Changed
Read More: X-Men Star Tyler Mane Reveals ‘Super-Rare’ Male Breast Cancer Diagnosis
Federal officials said they reviewed a broad range of scientific evidence when updating the nation's dietary recommendations.
New dietary guidelines released in January marked a significant shift in alcohol messaging. Rather than recommending specific daily limits, the guidance now advises Americans to “consume less alcohol for better overall health.”
According to HHS, the recommendation was based on a separate scientific review rather than the SAMHSA-led report.
US FDA Approves First New Sunscreen Ingredient Since the 1990s

Credit: Canva
For the first time in 20 years, the US Food and Drug Administration (FDA) has added bemotrizinol to the list of permitted sunscreen active ingredients.
Bemotrizinol is the first new active ingredient added to the over-the-counter (OTC) sunscreen monograph since the late 1990s and has been used for years in Europe and Asia.
“As promised in the Trump Administration’s MAHA Strategy Report, HHS is advancing innovation by bringing a new sunscreen ingredient to the US market for the first time in 20 years,” said HHS Secretary Robert F. Kennedy Jr.
“Bemotrizinol has been used safely in Europe for decades, and FDA’s action will increase competition and consumer confidence in sunscreen products.”
On December 11, 2025, the FDA proposed allowing the use of bemotrizinol in sunscreens. The agency finalized the action within seven months of issuing the proposed order.
Bemotrizinol is known to provide stable, long-lasting protection against both types of ultraviolet (UV) rays that can damage the skin. According to the FDA, it is also gentle enough to be used safely by young children.
What Is Bemotrizinol?
Also read: X-Men Star Tyler Mane Reveals ‘Super-Rare’ Male Breast Cancer Diagnosis
Bemotrizinol, also known as BEMT, is a chemical sunscreen filter that absorbs both UVB and UVA rays. The sun emits ultraviolet radiation, which sunscreen products are designed to block.
UVA and UVB rays affect the skin differently. UVA rays are primarily associated with tanning and skin ageing, while UVB rays are more closely linked to sunburn. UVB rays can also be partially blocked by barriers such as windows and clouds.
According to the University of Texas MD Anderson Cancer Center, about 95 per cent of the UV radiation reaching the Earth's surface is UVA, while UVB accounts for the remaining 5 per cent.
Sunscreens protect the skin either by creating a physical barrier using mineral ingredients or by using chemical filters that absorb UV radiation before it reaches the skin. Bemotrizinol belongs to the latter category.
The addition of BEMT is being welcomed by many experts because options that are both highly effective and considered safe remain limited in the US sunscreen market, according to an annual report by the Environmental Working Group (EWG), a nonprofit health and environmental advocacy organization.
Why Is Bemotrizinol Considered Beneficial?
Read More: Confused By Your Cholesterol Report? Here's What LDL And ApoB Really Mean
Bemotrizinol offers several characteristics that make it an effective sunscreen ingredient. It provides broad-spectrum protection against both UVA and UVB radiation and can achieve higher SPF protection at lower concentrations than some other commonly used sunscreen chemicals, according to Certified Laboratories and the FDA.
The ingredient is also photostable, meaning it breaks down more slowly when exposed to sunlight, helping maintain protection for longer periods. Because it is oil-soluble, it can be easily incorporated into creams and lotions.
In addition, bemotrizinol is minimally absorbed through the skin and rarely causes irritation, which is one reason the FDA considers it safe for use in children as young as six months old.
Bemotrizinol Added to OTC
Meanwhile, DSM Nutritional Products, a manufacturer submitted an OTC monograph order request seeking to add bemotrizinol, marketed as Parsol Shield, at concentrations of up to 6 per cent as a new active ingredient in the OTC sunscreen monograph.
“The FDA reviewed the request and proposed to amend the OTC monograph to add bemotrizinol as a sunscreen active ingredient,” the agency said in its announcement.
In December 2025, DSM had announced that, once approved, Parsol Shield would be available for use in sunscreen products in accordance with the monograph requirements.
According to the FDA, OTC monograph drugs such as sunscreens can enter the market without an approved drug application if they meet specific requirements, including permitted active ingredients, uses and dosage limits established under the monograph.
The FDA can modify an OTC monograph through an administrative order, and manufacturers can initiate the process by submitting an OTC monograph order request.
Raghu Ram Celebrates 10 Years Of Smoking-Free Life: Here's How He Did It

Raghu Ram took to Instagram to share anecdotes from his journey. (Photo credit: AI generated)
Remember Raghu Ram from the MTV reality show 'Roadies'? The actor and television host recently celebrated 10 years of a smoke-free life and took to Instagram to share his progress with fans. Smoking is injurious to health, and that is a known fact. It is associated with heart disease, cancer, hypertension, and even respiratory difficulties in the future. This habit can turn fatal too if one becomes addicted to nicotine. But for Raghu Ram, this journey ended 10 years ago, and he has never looked back since.
From chain smoker to now
"Iss mahine cigarette chhodkar mujhe pure 10 saal ho gaye hain. Or main aisa waise smoker nhi tha. Main peeta tha din mein 1-2 packets daily. Yani 20-40 cigarettes roz. Par maine bahut koshish ki chhodne ki, lekin addiction hoti hai, chor nhin pate hain log. Main bhi nhin chor paya tha," Raghu said in an Instagram video.
"Aisa chora ki wapas ek bhi kash nahin mara. 10 saal ho gaye hain mereko," he added.
How did Raghu Ram quit smoking?
On his podcast Mencyclopedia in 2023, Raghu Ram revealed that he once smoked 20–40 cigarettes a day for 15 years and then suddenly stopped.
"I smoked 20–40 cigarettes every day for 15 years, and then I just stopped. Cold turkey. And I had not taken a puff of a cigarette in 7 years," he said in his podcast titled How I Won the Longest Battle with My Addiction.
After trying several times to quit, Raghu Ram finally gave up smoking after marrying his wife, Natalie Di Luccio, a Canadian singer, in 2018.
Raghu Ram's 7-step guide to quitting smoking
Here is a simple seven-step guide from the former 'Roadies' host and judge:
- Decide on a date when you want to quit smoking and announce it to everyone.
- Overdo it a day or two before that so that you are fully disgusted by the act.
- List all your smoking triggers in order of severity.
- Avoid situations that can trigger you during the initial phase when you are struggling with withdrawal symptoms.
- Once you are through the first two weeks, you can gradually put yourself in trigger situations—from least to most severe—and still manage to resist the urge to smoke. Exercise regularly, as it makes a significant difference to your cravings.
For every person who has ever quit smoking or wanted to do it
For everyone who has ever quit smoking, the reasons may look different, but they all have two things in common: first, an addiction they are battling; and second, withdrawal symptoms to overcome. You may not be able to follow Raghu Ram's seven-step guide exactly, but his story is inspiring enough to encourage people to try quitting smoking.
© 2024 Bennett, Coleman & Company Limited

