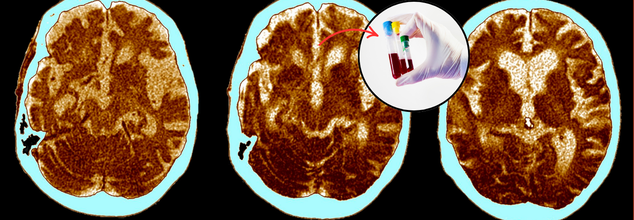
No More Brain Scans Needed, A Simple Blood Test Could Identify Alzheimer’s At Any Stage
In a monumental scientific finding researchers have developed an experimental blood test that not only detects Alzheimer's disease but can follow track its progression with remarkable accuracy, providing a historic advancement in Alzheimer's diagnostics and research. Published in Nature Medicine, the research is promising hope for millions across the globe by suggesting a less expensive, quicker, and more straightforward substitute for old diagnostic devices.
Alzheimer's disease has long defied early and conclusive diagnosis. Now, brain scans and spinal taps are the gold standards, but these procedures are expensive, invasive, and frequently out of reach—particularly outside of large urban or research centers. The recently discovered blood test could fundamentally transform that situation.
Scientists at Washington University School of Medicine in St. Louis have homed in on a blood protein known as MTBR-tau243, which is highly linked with tau tangles in the brain—a signature of Alzheimer's disease pathology. These tangles usually form after amyloid plaques, a key point in disease development when cognitive symptoms start to emerge.
This blood test definitively detects Alzheimer's tau tangles, which is our best biomarker measure of Alzheimer's symptoms and dementia," says Dr. Randall Bateman, co-senior author of the study and professor of neurology at Washington University.
The researchers initially discovered robust relationships between MTBR-tau243 levels in spinal fluid and the occurrence of tau tangles. They then went on to do the same, but with a much less intrusive method using blood samples. In their analysis, they used 108 U.S. and 55 Swedish patients and validated them using an extra cohort of 739 individuals.
Recruits spanned several levels of cognitive impairment—from presymptomatic subjects with higher amyloid load to those having frank Alzheimer's dementia. Critically, subjects with other causes of cognitive impairment were also recruited to evaluate test specificity.
The findings were dramatic: the blood test showed 92% specificity in detecting tau tangles, with protein rising steadily as dementia worsened. MTBR-tau243 was as much as 200 times higher in those with Alzheimer's dementia than in those who had only mild impairment.
Most hopefully, MTBR-tau243 levels were normal in those with non-Alzheimer's cognitive problems and in those with amyloid deposits but without symptoms—emphasizing the test's specificity in singling out genuine Alzheimer's cases.
This diagnostic innovation is not just a device—it may be a doorway to tailored care. As more Alzheimer's therapies become available, such as medications that attack either amyloid or tau proteins, identifying a patient's individual disease stage becomes essential to customize treatments.
We're on the verge of the age of personalized medicine for Alzheimer's disease," says co-lead author Dr. Kanta Horie. "When we have a clinically available blood test for staging, along with treatments that are effective at various stages of the disease, physicians will be able to tailor their treatment regimens to the individual needs of each patient.
For instance, anti-amyloid treatments would perhaps be most effective in the early phases where tau tangles are not very extensive. However, more developed phases characterized by massive tau deposition could be treated with anti-tau drugs or newer combination drugs being explored.
What Happens to the Brain in Alzheimer's Disease?
Alzheimer's disease is a progressive neurodegenerative illness that gradually erodes memory, thinking ability, and eventually, the capacity to perform everyday tasks. Essentially, the disease interferes with the brain's basic biology.
The healthy brain has tens of billions of neurons that exchange information through electrical and chemical signals. These signals travel through complex networks that include dendrites (which receive messages), cell bodies (which contain genetic material), and axons (which send messages to other neurons).
Alzheimer's interferes with these fundamental processes. Amyloid plaques first appear between neurons and then tau tangles within them. The outcome is disrupted communication, cellular metabolic breakdown, and collapse in mechanisms to repair the brain. Gradually, critical parts of the brain like the hippocampus and cerebral cortex become badly damaged, disrupting memory, language, judgment, and behavior.
While some brain shrinkage is natural with age, the extensive loss of neurons in Alzheimer's is much more crippling. Eventually, the disease causes death, with patients losing their self-sufficiency many years before they succumb.
Will this Blood Test Simplify Alzheimer's Care?
With close to 55 million individuals across the globe already living with dementia—and Alzheimer's responsible for 60–70% of all cases—the worldwide burden is staggering. Delays in diagnosis routinely preclude early intervention, multiplying the emotional and financial cost for families and healthcare systems as well.
This blood test is scalable. It could be used in primary care clinics, rural healthcare facilities, and low-resource nations—places where sophisticated imaging technology and neurologists might be scarce.
By streamlining diagnosis and allowing for earlier detection, the test not only empowers doctors but also provides patients and families with a greater opportunity for planning, symptom management, and participation in clinical trials or therapies based on their disease stage.
Although the blood test remains in the experimental stage, the pace is developing strongly. With more validation and regulatory endorsement, MTBR-tau243 testing may become standard procedure in Alzheimer's screening protocols in the near future.
For the time being, it is a significant scientific achievement—a hope beacon in the extended, protracted battle against Alzheimer's. While we make slow but certain strides toward solving the brain's enigmas, instruments like this put us a step closer toward a time when Alzheimer's can be found early, controlled with ease, and, one hopes, prevented entirely.

Image Credits: Canva
Man Dies From Brain Damage After Drinking Just One Sip Of Rotten Coconut Water
What was meant to be a refreshing drink from a tropical delight became a medical disaster for a 69-year-old man in Aarhus, Denmark. Following the ingestion of only a small quantity of coconut water from a rotten coconut, the man developed sudden onset of severe symptoms that resulted in his death within 26 hours of admission. This startling case, reported in a recent scientific study and widely debated in the international medical community, highlights a lesser publicized but potentially deadly foodborne hazard- fungal neurotoxins.
This is not merely an isolated event—this is a wake-up call for consumers and food safety agencies around the world, especially as pre-packaged and fresh fruits and vegetables become increasingly popular in home kitchens as well as tourist destinations.
The Danish man, whose name has not been released, bought a pre-hydrated coconut about a month ago. Left at room temperature on his kitchen table, the coconut had obviously spoiled. When he drank the water through a straw, the man quickly detected a bad flavor and discarded the coconut after examining its slimy, rotten center. Sadly, that one sip was enough.
Within a span of three hours, the man came down with a high fever, profuse sweating, and vomiting. Emergency workers encountered him pale, confused, and unbalanced—symptoms indicative of acute neurological distress. He was taken to the hospital, where an MRI confirmed massive brain swelling. Despite intensive treatment and a diagnosis of metabolic encephalopathy (a state in which the brain is impaired by chemical imbalances), his condition quickly deteriorated. He was pronounced brain dead just more than a day later.
Ssuspicions fell initially on the known food toxin bongkrekic acid, but continued study and tests revealed a sinister culprit: a fungus, Arthrinium saccharicola, in the man's windpipe and also in the rotting coconut.
This is a rare fungus, which produces 3-nitropropionic acid (3-NPA), an agent that is known to be highly neurotoxic. The toxin has the effect of breaking down the production of cellular energy in the brain, causing rapid swelling, loss of brain function, and death in extreme conditions. Importantly, there is no antidote for 3-NPA; supportive treatment is only offered, and this is centered on symptom management like encephalitis, seizures, and metabolic imbalance.
What's even more worrisome is that it wasn't much coconut water that triggered this effect. It only needed an infinitesimal dose of the toxin from the fungus to be devastatingly detrimental to the brain.
The toxicity of 3-NPA is not new. Chinese and some African medical journals have reported poisonings since the early 1990s. In all such cases, moldy sugarcane was the source. Patients experienced gastrointestinal upset—vomiting and diarrhea—followed by neurological symptoms such as confusion, seizures, and coma. In some cases, the illness was fatal.
This Danish case is the first reported instance linking Arthrinium saccharicola to spoiled coconut water, and as such, it is a highly unusual and alarming case of how this toxin can appear from various food sources based on storage and environmental conditions.
Why Refrigeration Isn't Optional for Food Safety?
Experts now want consumers to rethink how they store coconuts and other perishable fruits. Dr. Samuel Choudhury, a Singapore-based medical influencer with more than 300,000 followers, stressed in an Instagram post the need to keep pre-shaved coconuts refrigerated. "Always keep these coconuts in the fridge since they are already partially peeled," he explained. "Only whole coconuts should be kept at room temperature."
The outer husk of intact coconut serves as a natural covering, slowing down spoilage. But when shaved or pierced, the exposed white interior becomes very vulnerable to microbial and fungal invasion. Left on the kitchen counter, these coconuts will ferment, spoil, or acquire toxic fungi—without any signs of mold or warning until too late.
Significance of Consumer Awareness
Although coconut water is touted for its hydrating qualities and is a common staple in most tropical diets, this particular instance points to the potential dangers of mishandled or stored improperly natural drinks. With the worldwide trend towards fresh, unprocessed foods, education for consumers becomes increasingly vital.
Health officials all over the world are taking heed. In the wake of the incident, European food safety networks have reaffirmed requiring explicit labeling of fresh coconut products, such as expiration dates and storage in refrigerators.
Even a sip of improperly stored coconut water can prove deadly due to rare fungal toxins. Always refrigerate partially peeled or pre-shaved coconuts, consume them within a few days, and discard anything that tastes or smells off. When in doubt—throw it out.
Credit: Canva
Australians Encouraged To Get Flu Shots As Temperatures Drop
Australian health authorities are encouraging residents to get their flu shot as cases surge nationwide, with one state seeing numbers nearly double. According to the National Notifiable Diseases Surveillance System, over 46,300 flu cases were recorded across Australia by the end of March this year—a rise of approximately 50 per cent compared to the same period last year. The data revealed that 67 people in Queensland had been hospitalised due to influenza, and 900 new cases were confirmed within a single week. Meanwhile, in Victoria, more than 10,000 flu cases have been reported so far, with numbers continuing to climb—almost double compared to the same time last year.
April Is The Right Time To Get Flu Shots: Authorities
It is pertinent to note that Australia is located in the southern hemisphere and is currently moving towards the much-dreaded winter season. While winters are not directly linked to influenza and related diseases, they create conditions that make it easier for flu viruses to spread and for people to become infected.Victorian Chief Health Officer Tarun Weeramanthri told the leading Australian news publication Nine, that April is the ideal time to get vaccinated before flu season peaks in June and July. "It does take a couple of weeks before those antibodies come into your body and give you that protection – so you'll get peak protection if you go out and get vaccinated now," he explained. A spokesperson from the Australian Health Department warned that the flu poses a serious threat to babies, young children, and those with underlying health conditions. Vaccination is available to everyone over six months of age.
“It can require hospitalisation and can cause death,” the spokesperson said. “Vaccination is a safe and effective way to protect yourself and your family from serious disease caused by influenza.”
Who Should Get Vaccinated?
The Australian Government recommends that everyone over the age of 6 months has an influenza (flu) shot every year. Categories which particularly need to get jabbed include children aged six months to five years, pregnant women, individuals over 65, and those with medical conditions.What Is Flu? What Are The Symptoms?
Flu, or influenza, is a contagious viral infection that targets the respiratory system of a person. However, many confuse it with the common cold. While flu and the common cold can have similar symptoms, like runny nose and cough. But cold symptoms are usually mild and flu symptoms can be severe and lead to serious complications. Different viruses cause colds and the flu.Key symptoms include:
- Fever
- Chills
- Cough
- Sore throat
- Stuffy nose
- Body aches
- Headaches

6 Test Positive For Measles In Texas As RFK Jr Touts Vitamin A As Possible Cure
Six young children at a Lubbock, Texas, day care center have tested positive for measles—a dreaded scenario with the potential to accelerate an already out-of-control outbreak that has spread to at least two other states. More than a dozen other states and Washington, DC are dealing with cases of measles unrelated to Texas. As per the Centres For Diseases Control And Prevention (CDC), 22 jurisdictions have been hit by measles as of now.
On Friday, the Texas Department of State Health Services said the toll rose to 481 confirmed cases, a 14% jump over last week. Fifty-six people have been hospitalized in the area since the disease started spreading in late January.
What Do We Know About The Case In Texas?
Measles outbreak in Texas began on March 24, when a little girl at Tiny Tots U Learning Academy, who had been sick with fever and vomiting tested positive. She later needed to be hospitalized for pneumonia and trouble breathing. Kids who have tested positive at the day care so far are between the ages of 5 months and 3 years old, said Maegan Messick, a co-owner of the center. None was fully vaccinated against measles.
For nearly two weeks, Messick has been working with local health officials who are in contact with the Centers for Disease Control and Prevention about the situation. Messick said she’s not been given clear guidance on how to handle measles in such a large day care with so many vulnerable kids. "From what I’m being told, the CDC doesn’t have a playbook for this," Messick said. "We’ve just had to make judgment calls."
How Is US Dealing With Measles?
Donald Trump lead US is facing the largest measles outbreak in six years, but the CDC has remained relatively silent on the public health threat, providing just weekly updates on its website and sending an alert to doctors last month. The agency sent 2,000 doses of the MMR vaccine to Texas health officials at their request but hasn't held a news briefing about measles since 2019, when two large outbreaks in New York threatened to reverse the United States’ status of having eliminated the virus.
RFK JR Suggests Vitamin A As Possible Treatment, Posioning Reported
Meanwhile, United States Secretary of Health and Human Services Robert F Kennedy Jr has touted Vitamin A as a potential treatment option against measles. For decades, RFK Jr has been openly discrediting vaccines, linking them to Autism and other diseases. On Friday, it was reported that children who were infected with measles and given Vitamin A in Texas were found to be suffering from liver toxicity. Speaking to USA Today, Dr Lara Johnson, a pediatric hospitalist and chief medical officer of the Covenant Health-Lubbock service area, stated that all the children underwent routine lab testing, which showed abnormal liver function believed to be caused by Vitamin A toxicity.
How To Identify Measles?
First symptoms show after 7–14 days after a measles infection. They include:
- High fever (may spike to more than 104°)
- Cough
- Runny nose (coryza)
- Red, watery eyes (conjunctivitis)
- 2–3 days after symptoms begin: Koplik spots
- Tiny white spots (Koplik spots) may appear inside the mouth two to three days after symptoms begin.
Measles rash appears 3 to 5 days after the first symptoms. It usually begins as flat red spots that appear on the face at the hairline. They then spread downward to the neck, trunk, arms, legs, and feet.
- Small raised bumps may also appear on top of the flat red spots.
- The spots may become joined together as they spread from the head to the rest of the body.
- When the rash appears, a person's fever may spike to more than 104° Fahrenheit.
© 2024 Bennett, Coleman & Company Limited

