- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
Do You Think You Have High Alcohol Tolerance? Here’s How Liquor Impacts Your Brain Activity

Liquor Impacting Brain Activity (Credit-Freepik)
Many of us believe that we are great drinkers and that alcohol does not affect us as much. People who are able to drink without showing any sign of inebriation are known as social drinkers. In short, they are not addicted to alcohol but will not turn down the opportunity to have a good time! While it may seem like it doesn’t affect you, new studies suggest that it is just an illusion, even if you have high tolerance, alcohol affects your cognitive and motor functions more than you think.
The study reveals the below implications and techniques:
- Researchers used a new MRI technique to precisely measure brain electrical activity.
- By comparing brain scans before and after drinking, scientists identified specific areas affected by alcohol and how much brain activity slowed down.
- Participants were chosen to be regular social drinkers without alcohol addiction, ensuring the study focused on the effects of alcohol alone.
- MRI technology provided reliable data on brain activity changes caused by alcohol consumption.
How does the brain react to alcohol?
The human brain is a complex network of billions of neurons that communicate through electrical impulses. Brain conductivity refers to the efficiency with which these electrical signals travel through brain tissue. It's akin to the speed and clarity of a digital signal through a wire. In layman terms, your brain must function in its peak condition as it is essential for various cognitive processes, including memory, attention, decision-making, and motor control.Think of it as the foundation for your brain's performance. When brain conductivity is high, information flows smoothly, and that helps your brain in rapid processing and response. On the other hand, low conductivity can hinder cognitive function, leading to slower thinking, impaired memory, and difficulties with coordination.
A study conducted at the Neuroscience Research Australia (NeuRA) and UNSW Science unveiled a startling connection between alcohol consumption and brain conductivity.
What is the connection between alcohol consumption and brain activity?
While many people brush off the effects of alcohol as temporary changes in behaviour, the reality is much more complex. Beyond the obvious impacts on coordination and judgment, alcohol significantly alters brain function. Alcohol dramatically slowed down brain activity, especially in areas responsible for decision-making, planning, and physical coordination. This decline was so significant that it resembled the brain changes seen in normal ageing. This means even one drink could temporarily accelerate the ageing process of your brain.
Alcohol and Brain activity: What does the study Imply?
The implications of this research are far-reaching. It provides compelling evidence that alcohol consumption has a direct and measurable impact on brain function. The discovery that alcohol can significantly reduce brain conductivity opens new avenues for understanding the neurocognitive effects of alcohol abuse and dependence. While you may not feel like alcohol is affecting you and you have a high tolerance, it most definitely changes and affects your decision-making abilities and impulse control.
Furthermore, the MRI technique employed in the study could be a valuable tool for assessing the impact of other substances on the brain and for developing interventions to mitigate alcohol-related brain damage.
Cancer Patients To Face Higher Costs As India Raises Chemotherapy Drug Prices Amid Nationwide Shortage
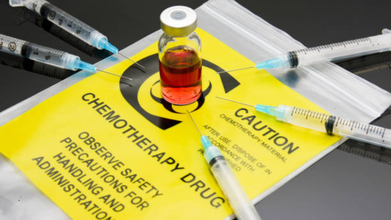
Credit: iStock
Cancer patients in India, already affected by shortages of critical chemotherapy drugs, are now set to face higher costs after the government approved a price hike.
Facing significant shortages are Cisplatin and Carboplatin — the two platinum-based drugs that form the backbone of treatment for common cancers such as oral cancer, breast cancer, ovarian cancer, cervical cancer, esophageal cancer, and testicular cancer.
Shortages Disrupt Cancer Treatment
The shortage of these essential chemotherapy medicines is disrupting care across hospitals and cancer centers, with several doctors pointing out that a substantial proportion of chemotherapy protocols for solid tumors rely on one of these platinum-based agents.
The drugs have been facing shortages as companies find it difficult to sustain production amid rising manufacturing costs linked to the ongoing conflict in the Middle East.
The two drugs, often prescribed in combination and with no alternatives, are derived from platinum, a precious metal whose cost has surged due to the Middle East conflict and the closure of the Strait of Hormuz.
Rising Production Costs Hit Manufacturers
Also read: India Revises Folic Acid Measurement Unit to Prevent Dosage Errors
"The production cost has increased because the API, or active pharmaceutical ingredient, which is imported from abroad, has become more expensive. As a result, manufacturing costs have gone up, but the MRP has not increased," Dr Shyam Agarwal, Senior Consultant, Medical Oncology at Sir Ganga Ram Hospital, told HealthandMe.
As companies have struggled to sustain production amid rising manufacturing costs, they approached the government seeking a revision of the price cap.
Drugmakers reportedly sought price revisions for 82 medicines, citing substantial increases in production costs due to the US-Iran conflict linked to the Hormuz crisis and other factors.
Government Approves Higher Prices
In response, the National Pharmaceutical Pricing Authority (NPPA), following permission from the Union government's Department of Pharmaceuticals (DoP), has increased maximum retail prices for four drugs, including the life-saving cancer medicines Cisplatin and Carboplatin, and two anti-tetanus injections.
While the move is aimed at restoring supplies, it has also raised concerns about affordability for patients already battling a costly disease.
The NPPA is the country's drug price regulator and functions under the DoP, Ministry of Chemicals and Fertilizers.
NPPA Asked to Review Cost Increases
Read More: India's Maternal Mortality Ratio Drops From 130 To 87 In Last 10 Years: Govt
The ministry directed the pricing authority to determine how much prices could be increased.
The formula suggested: "The Standing Committee recommended a 10 per cent increase per year from the last fixation with a ceiling of 50 per cent, which could also be a guide, but the primary principle should be cost increase," News18 reported.
The DoP has further advised the NPPA to examine increases in raw material costs for these drugs while determining any price revisions. It has also asked the regulator to assess similar requests from the pharmaceutical industry, where price hikes have been sought due to higher raw material costs.
India Revises Folic Acid Measurement Unit to Prevent Dosage Errors

Credit: iStock
India's Ministry of Health has notified an amendment to the Drugs Rules, 1945, replacing the unit of measurement for folic acid under Schedule V from "mg" (milligrams) to "mcg" (micrograms).
The amendment has been brought into effect through the Drugs (Fourth Amendment) Rules, 2026, notified vide Gazette Notification G.S.R. 444(E) dated June 1, 2026. The notification will come into force after six months, according to the Ministry.
The move aims to avoid unnecessary confusion, reduce the chances of misinterpretation, and prevent incorrect administration of dosages of vitamin B9 — essential for the production of healthy red blood cells, especially during pregnancy.
The change follows the publication of draft rules in January 2026 and consideration of objections and suggestions received from stakeholders.
What Does The New Notification Say?
Also read: India Makes Significant Progress In Maternal Care, Nutrition And Child Immunization: NFHS-6
As per the notification, in Schedule V of the Drugs Rules, 1945, under paragraph 2 relating to standards for patent or proprietary medicines, the entry against "Folic acid" in the unit column has been amended. The earlier unit "mg" has now been substituted with "mcg".
The amendment will correct the unit of measurement, bringing it in line with internationally accepted dosing standards for folic acid, which is routinely prescribed and labelled in micrograms. This correction is also important because lower doses of folic acid are used prophylactically in situations such as pregnancy to prevent infant malformations. Higher doses, however, may be used to address specific conditions such as neural tube defects, Medical Dialogues reported.
The Ministry stated that the amendment has been made after consultation with the Drugs Technical Advisory Board (DTAB) and in exercise of the powers conferred under Sections 12 and 33 of the Drugs and Cosmetics Act, 1940.
According to the notification, the Drugs (Fourth Amendment) Rules, 2026, will come into force six months from the date of publication in the Official Gazette, giving manufacturers and other stakeholders sufficient time to make necessary compliance-related changes in product documentation, labelling, and regulatory records.
Why Is Folic Acid Important?
Read More: Introducing Eggs Before Age One May Lower Allergy Risk by 17%: Study
According to the American College of Obstetricians and Gynecologists (ACOG), folic acid is one of the most important nutrients in prenatal vitamins. This B vitamin helps create the baby's neural tube — the structure that eventually forms the brain and spinal cord.
Beyond pregnancy, people who do not consume enough folate- or folic acid-rich foods may develop folate deficiency. People with celiac disease and inflammatory bowel disease, which prevent the small intestine from absorbing nutrients properly, may also have low folate levels, as per the Mayo Clinic.
Folate is found mainly in
- dark green leafy vegetables,
- beans,
- peas,
- nuts.
Fruits rich in folate include
- oranges,
- bananas,
- melons,
- papayas.
The recommended daily amount of folate for adults is 400 micrograms (mcg). People who are planning a pregnancy or could become pregnant should get 400 to 800 mcg of folic acid daily.
Importantly, taking too much folic acid, especially over 1,000 mcg daily without a doctor's advice, can mask a vitamin B12 deficiency, potentially causing irreversible nerve damage and may lead to side effects such as bitter taste, nausea or sleep problems, with potential links to increased risks in pregnancy like autism or insulin resistance.
Dog Owners Likely To Be Happier Than Cat Lovers: Survey

Lifestyle choices influence long-term health, and pets might just be one way to achieve them. (Photo credit: AI generated)
In 2018, the General Social Survey (GSS)—a measure of American social and lifestyle trends—added a new subject to its agenda: pet ownership. The questions initially seemed light-hearted at first glance, but the findings noted that the relationship between health, pets, and overall well-being is noteworthy. The survey also found that approximately six in 10 American homes own pets, and this led researchers to explore how pet ownership affects social connection, lifestyle, happiness, and mental and physical health.
How does dog ownership affect mental health?
On a broader level, it was found that pet owners and non-pet owners report similar levels of happiness. More than 30 per cent of both groups described themselves as very happy, while a smaller group reported not being too happy. A closer look at the specific types of pet ownership showed a striking difference, however. Dog owners are twice as likely to be happy as cat owners. People who owned both dogs and cats were somewhere in the middle. Dog owners appeared to be happier than people with no pets, while cat owners, on the other hand, reported lower levels of happiness on average.
The survey revealed that the gap is noteworthy. The difference in happiness levels between cat and dog owners was larger than the gap between people who identified as middle class and upper class and nearly as large as the difference between people reporting fair health and those who described their health as good or excellent. The findings, however, did not prove that owning a dog can directly cause greater happiness.
Read more: Power Of Pets: Expert Explains The Science Behind Why Pets Make Us Happy
Why are dog owners likely to be happier?
The findings, however, do not prove that owning a dog leads to happiness. Researchers noted that other factors could also be responsible for this. For example, dog owners are more likely to be married and also homeowners—factors linked to emotional well-being and higher life satisfaction. Furthermore, evidence found that dogs contribute to a healthier lifestyle that supports mental and physical health.
Another significant benefit is physical activity. According to a 2013 study, dog owners are more likely to spend time outdoors and engage in regular exercise because daily walks and pet-related activities can improve sleep quality and heart health, lower stress levels, and reduce the risk of chronic diseases. These benefits can enhance quality of life and mood. Dogs may also encourage stronger social connections, as owners are likely to engage with strangers and neighbours, creating opportunities for conversation and friendship. Social relationships are a predictor of mental well-being and are linked with a lower risk of depression, loneliness, and anxiety.
The emotional bond between pets and people is another key factor for consideration. The GSS found that dog owners were more likely to play with their pets and seek comfort from them during difficult times. These interactions reduce feelings of isolation and help people cope with stress.
Read more: Pets Can Affect Your Mental Health As Much As Your Partners, Study Finds
The impact of cat ownership on health
Research on cat ownership found that cats can help reduce negative emotions and offer companionship, especially for quieter people with more independent relationships with pets. However, these benefits do not always translate into higher reported levels of happiness. Personality differences can also play a role here. Studies have found that dog owners are more socially engaging and extroverted, as opposed to cat owners, who are more introspective and independent.
Conclusion
The relationship between health and pets is intricate. Happiness and mental well-being can be influenced by several factors, including financial stability, physical health, relationships, and personality traits. However, evidence suggests that pets such as dogs can promote healthier behaviours and more fulfilling lives.
© 2024 Bennett, Coleman & Company Limited

