Credit: Canva
Australians Encouraged To Get Flu Shots As Temperatures Drop
Australian health authorities are encouraging residents to get their flu shot as cases surge nationwide, with one state seeing numbers nearly double. According to the National Notifiable Diseases Surveillance System, over 46,300 flu cases were recorded across Australia by the end of March this year—a rise of approximately 50 per cent compared to the same period last year. The data revealed that 67 people in Queensland had been hospitalised due to influenza, and 900 new cases were confirmed within a single week. Meanwhile, in Victoria, more than 10,000 flu cases have been reported so far, with numbers continuing to climb—almost double compared to the same time last year.
April Is The Right Time To Get Flu Shots: Authorities
It is pertinent to note that Australia is located in the southern hemisphere and is currently moving towards the much-dreaded winter season. While winters are not directly linked to influenza and related diseases, they create conditions that make it easier for flu viruses to spread and for people to become infected.Victorian Chief Health Officer Tarun Weeramanthri told the leading Australian news publication Nine, that April is the ideal time to get vaccinated before flu season peaks in June and July. "It does take a couple of weeks before those antibodies come into your body and give you that protection – so you'll get peak protection if you go out and get vaccinated now," he explained. A spokesperson from the Australian Health Department warned that the flu poses a serious threat to babies, young children, and those with underlying health conditions. Vaccination is available to everyone over six months of age.
“It can require hospitalisation and can cause death,” the spokesperson said. “Vaccination is a safe and effective way to protect yourself and your family from serious disease caused by influenza.”
Who Should Get Vaccinated?
The Australian Government recommends that everyone over the age of 6 months has an influenza (flu) shot every year. Categories which particularly need to get jabbed include children aged six months to five years, pregnant women, individuals over 65, and those with medical conditions.What Is Flu? What Are The Symptoms?
Flu, or influenza, is a contagious viral infection that targets the respiratory system of a person. However, many confuse it with the common cold. While flu and the common cold can have similar symptoms, like runny nose and cough. But cold symptoms are usually mild and flu symptoms can be severe and lead to serious complications. Different viruses cause colds and the flu.Key symptoms include:
- Fever
- Chills
- Cough
- Sore throat
- Stuffy nose
- Body aches
- Headaches
Credit: Canva
Measles Case In US Double Of 2024-Should You Get Measles Vaccine Now?
US now has more than double the number of measles cases it saw in all of 2024, with Texas reporting another large jump in cases and hospitalizations on Friday. Other states with active outbreaks — defined as three or more cases — include New Mexico, Kansas, Ohio and Oklahoma. The virus has been spreading in undervaccinated communities, and since February, two unvaccinated people have died from measles-related causes.
Measles is caused by a highly contagious virus that's airborne and spreads easily when an infected person breathes, sneezes or coughs. It is preventable through vaccines and has been considered eliminated from the U.S. since 2000.
The multi-state outbreak confirms health experts' fears that the virus will take hold in other U.S. communities with low vaccination rates and that the spread could stretch on for a year. The World Health Organization said last week that cases in Mexico are linked to the Texas outbreak.
Do you need an MMR booster?
The best way to avoid measles is to get the measles, mumps and rubella (MMR) vaccine. The first shot is recommended for children between 12 and 15 months old and the second between 4 and 6 years old.
People at high risk for infection who got the shots many years ago may want to consider getting a booster if they live in an area with an outbreak, said Scott Weaver with the Global Virus Network, an international coalition. Those may include family members living with someone who has measles or those especially vulnerable to respiratory diseases because of underlying medical conditions.
Adults with “presumptive evidence of immunity” generally don’t need measles shots now, the CDC said. Criteria include written documentation of adequate vaccination earlier in life, lab confirmation of past infection or being born before 1957, when most people were likely to be infected naturally.
A doctor can order a lab test called an MMR titer to check your levels of measles antibodies, but health experts don't always recommend this route and insurance coverage can vary. Getting another MMR shot is harmless if there are concerns about waning immunity, the CDC says.
People who have documentation of receiving a live measles vaccine in the 1960s don’t need to be revaccinated, but people who were immunized before 1968 with an ineffective measles vaccine made from “killed” virus should be revaccinated with at least one dose, the agency said. That also includes people who don’t know which type they got.
Credit: Canva
FDA Delays Approval Of Novavax COVID-19 Vaccine
The U.S. Food and Drug Administration (FDA) has postponed granting full approval to Novavax’s COVID-19 vaccine. The decision, which was anticipated by April 1, has been deferred as the agency says it requires additional information before proceeding.
While the Novavax vaccine is currently available under emergency use authorization, full approval by the FDA would pave the way for broader use and potentially reassure individuals seeking alternatives to mRNA vaccines, according to CNN.
This delay coincides with efforts by Republican lawmakers in at least seven U.S. states to restrict or ban mRNA vaccines. As reported by KFF Health News, some of these legislators are also urging federal regulators to revoke approval for mRNA-based COVID vaccines—shots that former President Donald Trump highlighted as a major achievement of his administration.
Unlike the mRNA vaccines developed by Pfizer and Moderna, Novavax uses a protein-based platform, a more traditional vaccine approach.
“As of Tuesday, April 1, we had responded to all of the FDA’s information requests and we believe that our [Biologics License Application] is ready for approval,” the company stated. Novavax added that the application “included robust Phase 3 clinical trial data that showed our vaccine is safe and effective for the prevention of COVID-19.”
The company also said it remains confident its “well-tolerated vaccine represents an important alternative to mRNA COVID-19 vaccines for the U.S.”
The delay follows leadership changes within the FDA. Dr. Scott Steele has been appointed acting director of the agency’s vaccine division after Dr. Peter Marks stepped down last month.
Meanwhile, U.S. Department of Health and Human Services (HHS) Secretary Robert F. Kennedy Jr.—a longtime vaccine opponent—has continued to circulate false claims about COVID vaccines and recently shared misleading information about the measles vaccine amid a deadly outbreak.
An HHS spokesperson told CNN that the FDA’s evaluation of the Novavax vaccine, like all vaccines, is undergoing an independent review process.
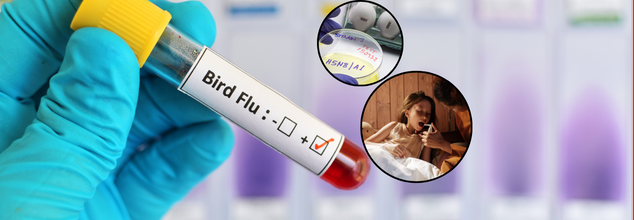
3-Year-Old Tests Positive For Bird Flu In Mexico- Experts Warn Of Rising Human Risk
In a case raising global public health concerns, a three-year-old girl from the western Mexican state of Durango has emerged as the nation's first officially confirmed human case of bird flu (H5N1), health officials announced on Friday. The case, combined with recent patterns of virus mutations, is highlighting increasing concerns among scientists globally that the avian influenza virus is moving closer to becoming a more general human threat.
The young girl, currently in serious condition at a hospital in Torreón, Coahuila, was diagnosed with the Type A H5N1 influenza virus, Mexico’s Health Ministry said in an official statement. While initially treated with antiviral flu medication, the severity of her symptoms prompted immediate hospitalization.
The question that still is not answered is how she became infected. Authorities initiated an investigation, screening wild birds in the area around her house, but no specific source has been confirmed. The Health Ministry stressed that the risk to the general population at present is still low. Nevertheless, the timing of the case—in the midst of growing H5N1 activity worldwide—is prompting greater alarm.
While H5N1 bird flu has been present in bird populations for decades, the last few years have produced a disturbing increase in its host range. In the United States alone, at least 70 people were infected in the last year, reports the World Health Organization (WHO), although experts estimate the true figure may be many times higher because of restricted testing and lack of reporting.
What was previously thought to be an avian-exclusive pathogen is now infecting an increasing band of species, small mammals, and, more recently, cattle. The virus's expanding capability for interspecies jumping dramatically increases the stakes for human health.
A new study by the University of North Carolina at Charlotte provides new evidence on why this outbreak—and future outbreaks—may become more deadly. Released in the peer-reviewed journal eBioMedicine, the research highlights how quickly the H5N1 virus is mutating to infect mammals and evade immune systems.
"The H5N1 virus is exhibiting evidence of enhanced adaptability to mammalian hosts, such as humans," explained lead author Colby Ford, a visiting scholar at the University of North Carolina Charlotte's Center for Computational Intelligence to Predict Health and Environmental Risks (CIPHER).
Ford and his colleagues employed powerful AI software to examine more than 1,800 virus-antibody interactions, targeting the hemagglutinin (HA) proteins—key molecules that enable the virus to infect host cells. The research discovered that newer virus variants have altered these proteins in ways that render them more evasive to current immune responses.
"This evolution makes previous infections and even current vaccines less effective," Ford said.
How the Virus Is Evading Human Immunity?
Perhaps the most dramatic revelation from the UNC Charlotte team was a dramatic mutation in a gene critical for the virus to infect mammalian cells and avoid immune detection. These mutations are making H5N1 transmit more easily—not only within bird flocks, but across species boundaries.
“High-performance computational modeling is helping us decode viral behavior at a much faster rate,” said CIPHER co-director Dan Janies. “We’re learning how the virus is shifting in real time and identifying key changes that could impact vaccine development and infection control.”
The speed and scope of the virus’s changes, Janies said, reinforce the urgency of proactive health measures rather than reactive responses.
Although the girl's case in Mexico appears to be an isolated incident, scientists warn that it could be the tip of the iceberg. As the virus becomes more effective at infecting mammals, such as livestock like cattle, the chances of human spillover events rise.
"Whenever a virus broadens its host range, it broadens its chance to mutate again," said Dr. Eleanor White, an international infectious disease expert at the Global Health Security Alliance. "Every new host is a possible lab for evolutionary change for the virus."
The fact that the girl's case took place in a non-agricultural environment, without a confirmed source, indicates environmental transmission is already occurring at a level health officials are not yet aware of.
The Mexico case has spurred demands for more intense surveillance, quicker diagnostic testing, and more comprehensive vaccine development programs that take into account viral evolution. It also underlines the need for global cooperation since viruses such as H5N1 have no borders.
"To avoid future outbreaks, we need to invest in visionary research, responsive systems, and public education," Ford emphasized. "The time is now—before a more virulent pandemic breaks out."
Public health professionals across the globe are called upon to keep close watch on livestock, wildlife, and human populations and remain open about reporting cases. Meanwhile, people are asked to keep their distance from ailing or deceased birds and report any strange animal behavior to the local authorities.
Although the risk to the general public is low at this time, the initial confirmed human case of H5N1 in Mexico, in addition to increasing studies on the virus's changing behavior, emphasizes a pressing need for caution. As the bird flu virus continues to become increasingly skilled at breaching species barriers, the world health community must get ready for a future in which H5N1 will no longer pose only a risk to animals—but to humans as well.
© 2024 Bennett, Coleman & Company Limited

